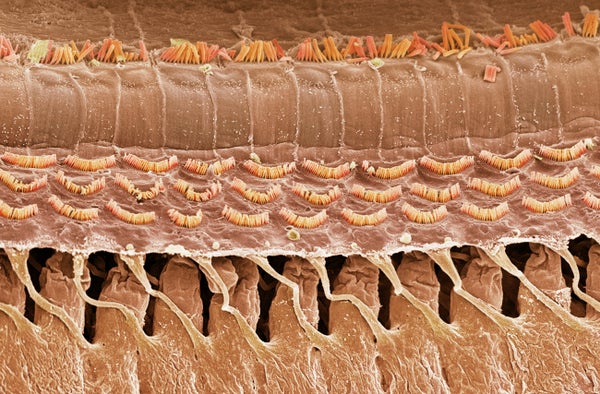
For decades the delicate and complex machinery of the inner ear refused to give up its secrets. The mystery related to how our ears convert mechanical energy from sound waves and head movements into electrical signals—an essential step in the process that creates hearing and balance.
The process, called transduction, occurs in other sensory systems as well. In vision, touch, taste and smell the pivotal molecules have been identified. But hearing proved more challenging. The inner ear is hard to reach and contains a fraction of the receptor cells of other systems. Auditory neuroscientists considered finding the protein at the heart of the transduction process the field’s “holy grail.”
As of this week the long quest is over. Researchers at Harvard Medical School report in Neuron that a sensor protein they had long suspected, transmembrane channel-like 1 (TMC1), was indeed essential for the conversion of sound or movement into electrical signals. “It answers a long-term question about how the hair cells in the inner ear actually work,” says David Corey, a neurobiologist at Harvard University and co-senior author of the new paper. “We had an idea that the TMC1 was fundamental, but we think our work really confirms that beyond any doubt.”
On supporting science journalism
If you're enjoying this article, consider supporting our award-winning journalism by subscribing. By purchasing a subscription you are helping to ensure the future of impactful stories about the discoveries and ideas shaping our world today.
When acoustic energy reaches the inner ear, it bends the tiny bundles of hair cells that line the snail-shaped cochlea; that movement sends electrical impulses to the brain. Working with mice, the Harvard team showed the TMC1 gene encodes a protein that forms a hole in the hair cell membrane to allow ions to pass through. That pore, known as an ion channel, serves essentially as a mechanical gate, opening and closing in response to sound. “TMC1 is the ion channel that actually does the job converting a sound stimulus into an electrical signal,” says Jeffrey Holt, an auditory neuroscientist at Harvard and co-senior author of the new paper. “It’s at the core of the process.”
Many in the field agree the results are conclusive, and all concur they are a significant advance. “This work is a real tour de force as far as basic biology goes, and it’s going to be a really important piece in moving forward to understanding various causes of deafness,” says Peter Barr-Gillespie, a professor of otolaryngology and director of the Hearing Restoration Project at Oregon Health & Science University who was not involved in the research. Although Barr-Gillespie says the work has just about convinced him of the central importance of TMC1, he nonetheless sees room for slivers of doubt. “I don’t think they 100 percent proved their case.”
After reading the study Stanford University neuroscientist Stefan Heller, who did not take part in the work, commented that the finding provides a critical addition to the picture of how the inner ear works: “We are finally at a point where the function of several members of the transduction machinery are being elucidated, and it will be important now to figure out how these individual parts work together and whether components are still missing. It is certainly an exciting time of critical discoveries about the biology of the senses of hearing and balance.”
The debate over TMC1 has been a long-running one. The gene was first identified in 2002 based on mutations in humans and mice that both led to deafness. (Some 2 to 8 percent of deafness cases are due to mutations in TMC1.) Scientists knew the gene played a role in transduction but the specifics were unknown. In 2011 Holt and colleagues hypothesized TMC1 might actually form the ion channel necessary for transduction. The new paper provides what Holt calls “smoking gun evidence” they were correct.
Corey, Holt, lead author Bifeng Pan and their colleagues have not yet determined precisely how TCM1 is structured. (That is on Barr-Gillespie’s wish list and is something Holt and Corey are working on now.) Instead, based on a series of biochemical experiments, they concluded TMC1 was probably a distant cousin of a different ion channel protein, TMEM16, about which far more is known. Using the structure of TMEM16 as a guide allowed them to make predictions about where to look in TMC1 for the pore. They then made targeted mutations in 17 different likely locations in the ears of neonatal mice to see if that changed the properties of the sensory hair cells. “We found that when we modified [the mutations], almost every one of them changed the way that ions go into the hair cell,” Corey says.
Beyond the advance in basic biology, these findings could indirectly lead to biological approaches to restore hearing. “As we start to understand how this whole thing assembles into a working system, then when any one part of it is broken, we have a better idea about how we might go in and fix it,” Corey says. Both Holt and Corey are working on gene therapies that either replace or repair genes causing hearing loss including TMC1. Other scientists are working on hair cell regeneration to treat acquired hearing loss using stem cells and other strategies.
Barr-Gillespie suggests a deeper knowledge of the transduction process might also prove helpful with hearing loss acquired from exposure to noise or ototoxic drugs—about half of the 460 million cases worldwide. “It’s pretty likely that the way in which the transduction machinery is maintained and put together and managed over the lifetime of an individual will impact age-related hearing loss as well,” he says.
Whereas identifying TMC1 is a critical step in understanding the molecular underpinning of hearing and balance, it is not the whole story. There is a chain of other proteins involved as well, and Corey and Holt are planning to attack those next. “It’s like fitting a big piece at the center of a jigsaw puzzle,” Corey says. “It should be much faster to see how the others go together.”