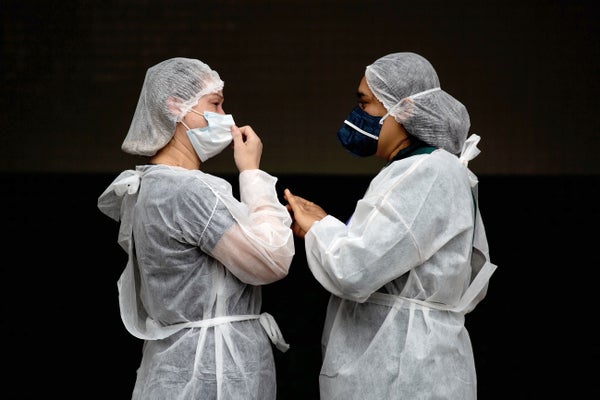
Manaus, a Brazilian city of more than two million that lies hundreds of miles from the Atlantic coast in the midst of the Amazon rain forest, has stood out as one of the world’s leading COVID hotspots. Tragically, it continues to provide the wrong lessons about what should be done to ease the spread of SARS-CoV-2, the virus that causes the disease.
The city and Brazil as a whole have become an exemplar of what happens when a country pursues a strategy of denying the pandemic and embracing herd immunity by letting the virus spread unchecked. Brazil’s president Jair Bolsonaro has promoted the idea of letting the pathogen move throughout the population until most people have been infected. He described proposals for a lockdown in Manaus before a crushing second wave of infections hit as “absurd.” And he has downplayed the severity of the crisis, saying that the nation of 211 million has to recognize that death is an inevitability and so Brazilians should stop being “sissies.” The country is currently recording around a quarter of all weekly COVID-19 deaths despite being home to less than 3 percent of the world’s population.
The legacy of the nation’s approach to countering COVID has meant that the spiraling case numbers and deaths registered in Manaus and the rest of Brazil are now spreading through the world in the form of a new variant of the virus. Studies suggest this variant could spread more than twice as fast. “Manaus was the first city to have its health system collapse in the new wave,” says Brazilian physician and neuroscientist Miguel Nicolelis. “But now there are many ‘Manaus’s all over Brazil’s five regions. Brazil badly needs help from the international community to handle this situation, or new variants from here will continue to spread worldwide!”
Manaus was devastated by a first wave of COVID cases beginning last March. Excess deaths—the 3,457 people in the city who died above the expected mortality figures between March 19 and June 24, 2020—represented 0.16 percent of Manaus’s relatively young population. And 7 percent of men older than 75 died at the peak of the spread.
Infections were so prevalent that researchers at the University of São Paulo and their colleagues concluded that Manaus was the first city in the world to reach herd immunity—the point at which enough people are immune to a virus that the spread of new infections is hindered. Their preliminary preprint study estimated that 66 percent of the population had been infected with SARS-CoV-2 (they later revised their figure to 76 percent as of October). The threshold for COVID herd immunity is unknown, but projections often cited range from 60 to 90 percent. Similarly high rates of infection have also been found in the Peruvian and Colombian Amazon.
After a peak of hospitalizations and deaths last April, numbers dropped to relatively low levels until November 2020, despite the reopening of schools and businesses. Some Brazilian researchers warned that the pandemic was not over. Infections could rise, and the absence of stricter public health measures would condemn the city to a resurgence. The response from public officials, they say, was always the same: herd immunity would protect them. This false sense of security precipitated the new wave of infections, says Jesem Orellana, a Manaus-based epidemiologist at the Oswaldo Cruz Foundation (Fiocruz), a leading Brazilian public health institute.
In December 2020 a second wave did hit. And by January the city’s health system, which serves communities across the Amazon, had collapsed. ICUs were full to bursting, and oxygen supplies became exhausted. Some patients were airlifted to other regions of Brazil. But many died of asphyxiation on makeshift beds in hospital corridors or their home, doctors say.
More severe than the first one, the new wave took Manaus by surprise. Wearing masks and practicing social distancing had been discarded in the belief the city had reached herd immunity. Caseloads surged out of control, and bleak milestones from last year were surpassed. In January alone more than 3,200 excess deaths were logged, Orellana says.
Questions arose as to whether herd immunity had ever been achieved, the number of people infected had been overcounted or immunity to the virus had waned. Another disturbing prospect was that mutations to the virus in the Amazonian city that had spawned what is called the Manaus variant, or more formally P.1, could have caused reinfections in people who had earlier bouts or could have sped the rate of transmission among the still uninfected.
“It’s quite hard to come up with any scenario that can be made to fit Manaus which is not hugely concerning,” says William Hanage, an epidemiologist at the Harvard T. H. Chan School of Public Heath.
Recent studies have corroborated the suspicions that P.1 drove Manaus’s second wave. The exact rate of infection prior to the recent upsurge has not been determined. But Hanage emphasizes that inducing immunity by leaving people to contract the virus unguarded is a mistake. “Following the tragedy of Manaus, I would hope we can put an end to discussion of controlling the pandemic through herd immunity acquired from natural infection,” he says.
Hanage hopes the dire scenes in the Amazon—hospital systems collapsing, grave diggers carving out trenches for mass graves shared by multiple bodies, and families desperately queuing for oxygen supplies—will send a clear message: “Herd immunity through infection, instead of a vaccine, only comes with an enormous amount of illness and death,” Hanage says.
“[People in Manaus] thought, ‘We passed through this big wave, so now it’s fine,’” says Paola Resende, a research scientist at the Laboratory of Respiratory Viruses and Measles at Fiocruz. “Of course, the people relaxed and started to live their life as normal. And of course, it happened again.”
Resistance to new measures persisted for months. Social distancing and mask wearing lagged. On December 26, 2020, when the state of Amazonas ordered businesses closed to slow rising infection numbers, protests by businesses and workers erupted, and the decision was quickly reversed.
The Manaus experience holds a cautionary message for the rest of the world, including the U.S., about maintaining basic public health strictures even as vaccination campaigns progress. And it underlines why only a global approach to immunizations will work.
“Manaus got hit really hard because they dropped all of their mitigations, and they didn’t have an adequate state of herd immunity,” says Warner Greene, a professor of medicine at the University of California, San Francisco, and founding director of Gladstone Institute of Virology and Immunology. “This false sense of security, it’s kind of like right now [in the U.S.],” he says. “I think we're gonna get hit really hard.”
Latin American countries—where vaccination numbers are behind the global North and infection rates are high—are fertile ground for breeding new variants. The more the virus spreads, the more it is able to find vulnerable groups in which mutations can arise.
The P.1 mutation is believed to have emerged in Manaus in early November 2020, but by January it made up three quarters of all variants detected in the city and had spread to Japan. It has since been detected in at least 34 other countries and regions, including the U.S. and the U.K. “We call [COVID] a pandemic because it’s everywhere,” Greene says. “And as long as it’s somewhere, it has the potential to be everywhere.”
Like other variants first detected in the U.K. and South Africa, P.1’s 17 mutations occurred unusually quickly, and many of them are in the spike protein, which is used to penetrate the cells of an infected person.
Research has not concluded that P.1 alone caused the crisis in Manaus despite previously high infection rates: overestimates of herd immunity or a natural decline in antibodies may be at fault as well. But there is mounting evidence that P.1 is more pernicious than its predecessors. A preprint lab study by the Brazil-U.K. Center for Arbovirus Discovery, Diagnosis, Genomics and Epidemiology (CADDE) estimated P.1 to be 1.4 to 2.2 times more transmissible than previous strains. And in another preprint paper, Fiocruz researchers found that the level of SARS-CoV-2, or viral load, in patients infected with the variant was 10 times higher.
More concerning is evidence that the Manaus variant is better able to evade antibodies. The same CADDE study estimated that P.1 dodges 25 to 61 percent of protective immunity gained from infection with earlier variants. There have been only three confirmed instances of P.1 reinfection, but cases are difficult to find and verify, Resende says.
Immunity gained through vaccination appears to be more robust than immunity achieved from infection. Though vaccines from leading manufacturers have generally shown less efficacy against P.1 than they have against older variants, Resende says that they still provide protection and that the issue should not yet ring alarm bells. Johnson & Johnson’s jab proved 85 percent effective against severe disease in trials in Brazil—no less than it did in the U.S.
Following P.1’s transmission across Brazil, infections are soaring nationwide. Most hospitals are operating at capacity, and 3,650 daily deaths were reported on March 26, the highest number to date. Two days earlier, the country’s total death count reached 300,000. P.1 may not only be driving higher infection rates in Brazil’s North Region, where P.1 is most prevalent. There is an increase in mortality in young people, suggesting it may cause more severe illness, says Margareth Portela, a senior researcher at Fiocruz.
Experts say that the situation is worrying—not just for the people of Brazil but for the rest of the world as well because of the virus’s track record of acquiring mutations in areas where it abounds.
The lingering concern is whether P.1 is a portent of what could happen if the pandemic continues unabated. It is not the only Brazilian variant. There is already a P.2. And the virus is continuing to alter itself in Brazil, deleting sites on the spike protein that antibodies bind to, according to preliminary research that has not yet been peer-reviewed.
Manufacturers are already working on how to tweak vaccines to account for new variants such as P.1, says Dan Barouch, an immunologist at Harvard University. But for now getting the existing ones rolled out as quickly as possible is key.
The U.S. is currently confronting the prospects of a vaccine surplus—and will have to decide what to do with the extra doses. “These viral variants provide a very strong argument for accelerating the vaccine campaign throughout the world because only with vaccination will we be able to control the pandemic and stop the emergence of new viral variants,” Barouch says. “And viral variants in the future, potentially, will be even more problematic than the ones we have today.”
Read more about the coronavirus outbreak from Scientific Americanhere. And read coverage from our international network of magazines here.