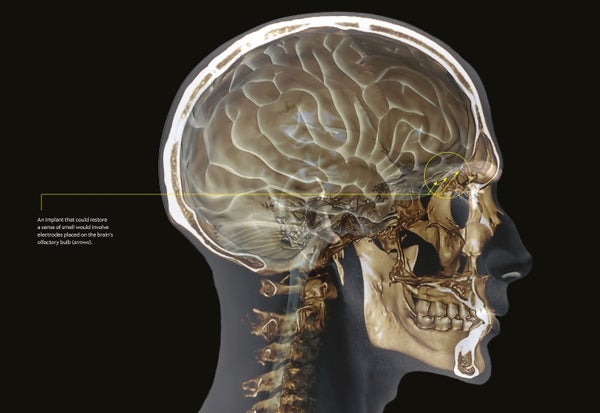
When Scott Moorehead tells people he cannot smell, they usually make a joke about how lucky he is—he must not be troubled by dirty diapers or people passing gas. “All the jokes are hilarious,” Moorehead says, with a hint of sarcasm. But his lack of smell also means he is vulnerable to natural gas leaks and burning food. He is self-conscious about his own scent, so he takes extra showers. And he has had to give up one of his favorite hobbies: matching wines with exotic flavors.
After a concussion left Moorehead without a sense of smell six years ago, these losses were all he could think about. “Just knowing that I was never going to be able to smell my wife again or my kids” was hard to cope with, he says.
Although the nerves that control smell can often regrow after an injury—they are some of the only neurons known to rapidly replace themselves—Moorehead's lesion was too severe. He now has anosmia, which means his sense of smell is gone. But he is participating in a nascent effort at the Virginia Commonwealth University (VCU) School of Medicine and Harvard Medical School to develop a partially implantable device that could help people with brain injuries decode and interpret everyday scents.
On supporting science journalism
If you're enjoying this article, consider supporting our award-winning journalism by subscribing. By purchasing a subscription you are helping to ensure the future of impactful stories about the discoveries and ideas shaping our world today.
Research on smell lags decades behind that on vision and hearing, says Joel Mainland, an olfactory neuroscientist and associate member of the Monell Chemical Senses Center in Philadelphia, who is not involved in the new work. Smell studies receive less funding than research on other senses does, he says. And smell involves many sensory components. Whereas vision requires interpreting input from three types of receptors, taste involves 40 and olfaction 400.
A surprisingly large number of people have an impaired sense of smell—23 percent of U.S. adults age 40 and older, according to one national survey, and 62.5 percent of those age 80 and older, according to another. Such a decline can result from injury, chronic sinus problems, genetics or aging, says VCU professor Richard Costanzo, who has studied smell for four decades and is co-leading the initiative to develop the new device. Often dismissed as inconsequential, smell contributes to taste, so people who cannot smell are at risk for malnutrition, as well as social isolation, Costanzo says.
Some smell-restoration treatments exist, Mainland says, including smell training, in which people repeatedly expose themselves to certain odors and practice identifying them. Other treatments may uncover specific causes of smell loss, such as chronic sinusitis. But for someone with the damage Moorehead suffered, none of these is effective.
Smell, like all senses, is a multistep process. Scents, technically called odorant molecules, enter through the nose or mouth and pass through a layer of mucus before binding to olfactory receptor neurons. This binding triggers electrical signals that reach certain spots in the brain's olfactory bulb. “One nerve cell may respond to a brownie but not to pound cake, and its neighbor might do the opposite,” says Eric Holbrook, chief of rhinology at Massachusetts Eye and Ear Hospital and an associate professor at Harvard Medical School. “One nerve cell probably responds to multiple chemicals, but they have some specificity.”
Holbrook, who is collaborating with the VCU team, is now trying to find a shortcut to stimulate the brain's olfactory bulb and then trigger a sensation of smell. Ultimately the researchers plan to create a device that will operate somewhat like a cochlear implant, an electronic device that partially restores hearing. Cochlear implants turn sounds into electrical signals that the brain interprets; in a similar way, the VCU-Harvard team hopes to convert chemical scents into useful electrical signals. Holbrook published a study in February in the International Forum of Allergy & Rhinology suggesting that electrical stimulation in the nasal cavity and sinuses can make a healthy person perceive an odor, even if it is not present. That is a long way from restoring a sense of smell in someone who has lost it, but it is an important step along the way, Holbrook says.
A cochlear implant has an external sound processor worn behind the ear that includes a microphone and microcomputer. That component transmits signals to an internal piece under the skin that stimulates nerves in the cochlea, the organ that converts sound vibrations into nerve impulses. Similarly, the VCU-Harvard team envisions a device that would potentially fit under the nose—or on a pair of glasses—and include an odor sensor and a small external microprocessor, as well as an internal part to stimulate different areas of the olfactory bulb, Costanzo says.
Daniel Coelho, a cochlear implant surgeon at VCU who is collaborating with Costanzo, says the researchers must still refine sensors so they can discriminate among enough odors to be useful. The plan is to miniaturize and expedite smell processing such as that carried out by so-called electronic noses, which are used for bomb detection and identification of spoiled food. In addition, researchers must determine the optimal surgical approaches to safely implant a device that can stimulate the brain to perceive smells.
Developing such an olfactory implant will take years, Coelho says, but it is not impossible. “It's a pretty straightforward idea. We're not inventing anything radically new,” he notes. Rather the team is putting existing technology together in a new way.
Moorehead, who injured himself falling off a skateboard while trying to teach his then six-year-old how to ride, is not optimistic about regaining his sense of smell. But he could not pass up the opportunity to help others, including the researchers. “It just kept seeming painfully obvious,” Moorehead says, “that this is what I'm supposed to do.”