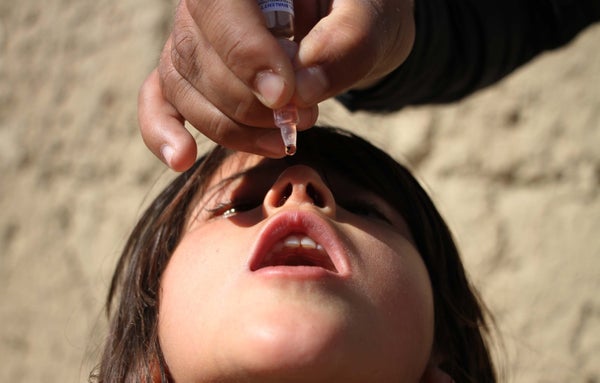
The year 2020 was on track to be a good one for South Sudan’s polio hunters. But now many of those working in the global polio eradication campaign are grappling with the potential reversal of much of their work. All house-to-house immunization efforts have been suspended because of the continuing coronavirus pandemic. Disease surveillance officers can scarcely travel at all. Polio samples awaiting testing are trapped in South Sudan because there are no flights to transport them to external laboratories, and local experts are bracing for the worst.
“The fact is, we cannot even move around anymore. This limits our action time,” says Sylvester Maleghemi, South Sudan polio team leader for the World Health Organization (WHO). “And this could overturn our work. But this is the reality of where we are right now.”
The worldwide polio eradication effort was suspended in late March, bringing campaigning to a near halt. More than 20 million doctors, technicians, and other medical and community practitioners have put much of their work on hold, leaving at least 13.5 million children unvaccinated or undervaccinated for polio so far, according to estimates by the public-private global health organization GAVI, the Vaccine Alliance. The WHO says that number could rise to at least 60 million by June in the eastern Mediterranean region alone (the area includes northern Africa, the Middle East and Central Asia).
On supporting science journalism
If you're enjoying this article, consider supporting our award-winning journalism by subscribing. By purchasing a subscription you are helping to ensure the future of impactful stories about the discoveries and ideas shaping our world today.
Yet even those figures mask the full extent of a disruption that could stifle polio eradication efforts for years, a dozen doctors, senior scientists and public health officials say. Millions of stored polio vaccine doses will lose their effectiveness if the pandemic prevents immunization for much longer, and some countries that are proceeding with limited vaccinations might run out before they can be resupplied. “If the lockdowns are in place for too long, then vaccines will just expire in many places,” says Thabani Maphosa, managing director of country programs at GAVI. “And we’re currently not able to get vaccines where we need to.”
Disease surveillance systems, which involve the collection and analysis of data on flare-ups so they can be suppressed, are a cornerstone of polio eradication. These systems are also wavering, in large part because of pandemic-related shutdowns and travel restrictions. When it comes to having the data or observations from the ground needed to keep polio in check, “you really don’t want to go blind. But we are seeing this generally across the board,” says Hamid Jafari, the WHO’s director of polio eradication for the eastern Mediterranean region. “Many health centers are closed. Patients are reluctant to seek help because they’re scared. Frontline workers are scared. And the severe restrictions on movement within [each] country make life difficult.”
Afghanistan and Pakistan, the two countries where wild polio remains endemic, largely rely on a “tiered” system for identifying the disease’s spread. This approach consists of community informers, frequent in-person visits to hospital pediatric wards and regular calls to local clinics to check for signs of acute flaccid paralysis—a rapid-onset weakening of respiratory muscles and other muscles that is associated with polio. But as the coronavirus pandemic advances and nations stall, these tiered networks are not functioning as they once did. In their reduced state, polio might gain a firmer footing.
And then there are the complications posed by thepolio immunizations themselves, which must be administered in several doses at different intervals. If too many areskipped, Maphosa says, “it’s a question, then, if it’s possible to catch up.” With roads still locked down in dozens of countries and polio teams unable to distribute vaccine stocks from central warehouses, many children are already missing doses—even when they are close at hand—according to GAVI.
The oral polio vaccine contains a weakened version of the virus, which is excreted in human waste. In rare cases in populations that are underimmunized, the weakened virus can mutate and infect nonimmunized people. It is too soon to determine if Niger’s recent outbreak of such “vaccine-derived polio” developed after the eradication campaign’s suspension. In any case, doctors anticipate an uptick in cases there and elsewhere over the coming months.
But in spite of these setbacks, the global polio program’s adaptability may actually have a silver lining for the current pandemic.
Retooling to Fight Coronavirus
Many countries have been quick to realize the usefulness of the polio network—the largest immunization program of its kind in the world—in fighting the pandemic. Much of the network has been redeployed accordingly.
Polio contact tracers, who are accustomed to searching out telltale signs of the disease such as sudden leg weakness, are now pursuing reports of severe respiratory distress, fever and other symptoms of COVID-19. “It’s a no-brainer, really,” says Maleghemi, who estimates that 80 percent of South Sudan’s polio personnel are nowtracking coronavirus cases themselves or training new tracers to do so where they cannot. “At a state level and county level, where we have the foot soldiers, everyone has been repurposed. If you go look for [acute flaccid paralysis], you can go look for [COVID-19].”
The polio network’s enormous infrastructure has been turned over to pandemic response in countries that have few other resources at their disposal. The WHO says Nigeria’s and Pakistan’s 24-hour emergency polio hotlines are now mostly dedicated to COVID-19, as are hundreds of labs andnetworks of country-wide cold freezer rooms and mobile units that normally store or transport polio vaccines.Once a vaccine is ultimately developed for COVID-19, the polio eradication teams are the ones most likely to support its distribution among the world’s less accessible areas, Jafari says.
Above all, the polio program contains considerable relevant technical expertise, which government officials in Somalia and Mali say has been instrumental in guiding their countries’ pandemic responses. Even though the parallels that can be drawn between the two diseases are limited, the basic principles are similar: case investigation, personal hygiene and patient isolation are vital. Disease surveillance is key, and it will become even more important if scientists find that water and wastewater analysis can yield the same kind of information for COVID-19 tracking as it does for polio. The WHO and the Bill & Melinda Gates Foundation are among those following up on promising early results.
Ultimately, however, polio teams will have to revert to their core mission. And when they do, they will face a rash of challenges.
Postpandemic Polio
Catching up on all those missed vaccine doses will be expensive—at a time when extra money is likely to be in short supply. The U.S. is the largest public funder of polio eradication. But the Trump administration has frozen its contribution to the WHO, through which much of the world’s polio aid is dispensed. Medical freight costs have already grown around 20 percent as a result of decreased air traffic, GAVI’s Maphosa says.
And the consequences of previous, much smaller disruptions to eradication efforts suggest polio teams will have a massive amount of damage to contain: In 2003 a single Nigerian state stopped vaccinating against polio for a year. This change fueled a resurgence in more than 20 countries, the WHO says.
In the long run, however, the pandemic-enforced stoppage may enable polio campaigners to reevaluate their approach, according to scientists at almost all the major polio partner organizations. After several disappointing years, during which the number of reported wild cases rose from an all-time low of 22 in 2017 to 176 last year, the polio teams need to take stock of past failures—and to refocus accordingly. If nothing else, they will likely begin again in a world more conscious of the perils of allowing health crises to fester.
“The polio program is sort of looking at this gap in our ability to actually implement [eradication efforts] to reexamine our strategies. And I think that, taking the long view, there’s been progressive success,” says Jay Wenger, head of polio eradication at the Gates Foundation. “It’s just been slow. And I think this gives us the opportunity to reevaluate what we really need to get done to finally finish the job.”
Read more about the coronavirus outbreak from Scientific American here. And read coverage from our international network of magazines here.