Companies and other players involved in the development of experimental Ebola drugs are jockeying to have their products tested in the outbreak in the Democratic Republic of the Congo, part of a chaotic and politically charged effort to use them in the midst of a crisis.
With one vaccine already being used in the field, plans are underway to see if another might also be tested. And as many as five drugs, most of which are not supported by much human data, could be used in head-to-head trials. When considering one of those treatments recently, scientific experts told the World Health Organization they couldn’t recommend its use at this time, but the DRC government has already said it’s eager to move ahead.
Experts say the maneuvering for space in which to try vaccines and drugs brings to mind the frantic days of the West African Ebola outbreak, when there were so many research teams in the field that a free-for-all of experimental testing ensued. Most of the clinical trials produced little in the way of insight into what actually might work against Ebola.
On supporting science journalism
If you're enjoying this article, consider supporting our award-winning journalism by subscribing. By purchasing a subscription you are helping to ensure the future of impactful stories about the discoveries and ideas shaping our world today.
There’s a “rush to evaluate [treatments] because the window of opportunity for evaluating these interventions is always going to be short,” said Ross Upshur, a physician and ethicist who was on the WHO panel.
There are “tensions” among organizations “that are rivalrous with each other,” not unlike the case in 2014, said Upshur, who is scientific director of Toronto’s Bridgepoint Collaboratory for Research and Innovation.
The final decision on which treatments to use rests with the government of the DRC. But the WHO expert panel has sought to provide guidance, and various nonprofits on the ground, particularly Doctors Without Borders, have their own views on the best course ahead.
Still, health officials say the crisis provides a crucial opportunity to better understand how to help contain outbreaks in the future.
“If we don’t use the opportunity to learn in this situation, we’ll never be able to know which is better than the other in terms of the drugs,” said Dr. Peter Salama, the WHO’s deputy director-general for emergency response.
Salama urged caution about the utility of experimental treatments, saying the efforts to use them will answer key questions about how feasible these therapies are in low-resource settings. “Everyone’s really excited about the use of these drugs, but are they useful in a rural African setting with very little infrastructure? The jury’s out,” he said.
Bikoro, one of two remote communities at the epicenter of the outbreak, has no power, no functioning lab, and very little infrastructure. The other, Iboko, is more remote and out of cellphone range. Health facilities in the region are rudimentary, and won’t easily lend themselves to the type of intensive care most of these therapies require.
“It’s not a simple effort to do this sort of trial in this kind of environment,” Salama said.
Three of the other experimental therapeutics are monoclonal antibodies—immune system warriors that can recognize and combat Ebola.
Two are cocktails that combine three antibodies—ZMapp, which was tested in West Africa, and a product made by Regeneron called REGN3470-3471-3479, which has already completed a small Phase 1 trial.
The third, called mAb 114, is being developed by the National Institute of Allergy and Infectious Diseases. It appeared to be efficacious in primate testing, but the Phase 1 study designed to determine if it’s safe to use and to establish the proper dosing only began on May 16.
The WHO expert panel advised against the use of mAb 114 in the outbreak response, given the limited data. But NIAID Director Dr. Anthony Fauci said he will send 100 doses of mAb 114, at the request of the DRC government.
DRC Health Minister Dr. Oly Ilunga told STAT in an interview that his government was “keen” to use it, nonetheless, because the treatment has its roots in his country’s third Ebola outbreak, in 1995 in the city of Kikwit.
The 114 antibody was isolated from the blood of a Kikwit survivor, and the DRC’s leading Ebola expert, Jean-Jacques Muyembe, collaborated with the NIAID on the research. Muyembe is the director general of the DRC’s National Institute for Biomedical Research.
“For us, it’s something very important, because the idea is derived from the research of a Congolese team with Dr. Muyembe,” Ilunga said.
There are two other drugs being considered for use in the outbreak—an antiviral called Remdesivir being developed by Gilead and a Japanese influenza antiviral known as favipiravir, which was tested in the West African outbreak.
A trial involving favipiravir failed to show it worked, and the WHO expert panel questioned the value of using it. But the fact that it is easier to administer than the others may improve its chances of being used.
The expert panel said ZMapp and Remdesivir ought to be the first and second choices, based on the available evidence.
Doses of ZMapp have already been shipped to the DRC, according to Larry Zeitlin, president of San Diegon-based Mapp Biopharmaceuticals. Although he would not specify how many doses were shipped, he said in an email that it was “more than they had asked for and we can resupply quickly and easily should it be needed.”
If ZMapp and Remdesivir aren’t available, the Regeneron cocktail could be used, the expert panel said. Leah Lipsich, Regeneron’s vice president for strategic program direction, said the company has “on the order of 100s of doses that would be ready to ship.”
The antibody therapies are delivered by infusion, which requires a level of patient monitoring that will be tough to achieve, Salama warned. And the Gilead drug requires daily kidney and liver function testing—also a challenge in these settings.
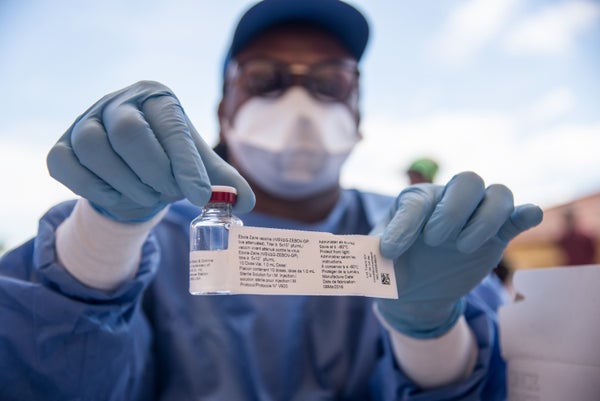
Vaccination of health care workers and people who have been in contact with Ebola cases—and contacts of the contacts—has been underway since May 21. This ring vaccination campaign, designed to prevent continued spread of the virus, has already vaccinated more than 400 people, Salama said.
The Merck vaccine is the only one that is currently being used in the ring vaccination program. But people are also eager to see if a second Ebola vaccine can be tested in this outbreak. This vaccine, made by Johnson & Johnson, requires two doses given one or two months apart—a drawback in an outbreak setting. Still, it’s believed the protection it triggers will last longer than that induced by the Merck vaccine.
The hope is that one day this vaccine, which is methodically making its way towards licensure, could be given to health workers throughout Africa’s Ebola zone. In the early days of Ebola outbreaks, health care workers are often among the virus’s victims, contracting the disease before it is recognized that Ebola is spreading.
Dr. Paul Stoffels, J&J’s chief scientific officer, said the company is exploring if there are ways to use its vaccine in the DRC in this outbreak.
“We are offering and we are evaluating options. The crisis is such that that is no place for politics and pushing,” said Stoffels, who noted J&J has 2 million doses of vaccine it could ship within a day or two of being asked. “We are open and ready to do whatever is needed.”
With the way the case counts look at the moment, that call may not come. Growth of the outbreak has slowed; the feared explosion of cases in Mbandaka—a city of over 1 million people—so far has not occurred. To date there have been 51 cases and 25 deaths. Nearly 90 percent of the cases have been in Bikoro and Iboko, a remote village inland from Bikoro.
If spread in Mbandaka has been halted, there may not be a way in for the J&J vaccine, Salama acknowledged.
“Is a trial actively being considered today? No. Is it a potential option at some point if the outbreak gets worse? Yes,” Salama said.
Republished with permission from STAT. This article originally appeared on May 30, 2018