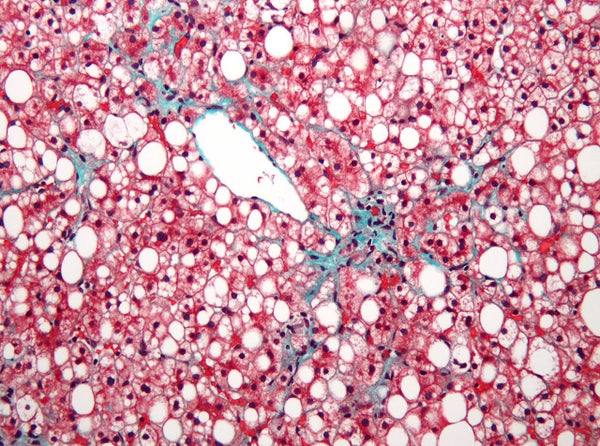
For most people, the acronym NASH won’t ring any bells. But NASH, or nonalcoholic steatohepatitis, is stealthily showing up in the livers of millions of Americans. Marked by the accumulation of an unhealthy amount of fat and scar tissue in the liver, NASH is quietly reaching epidemic proportions across the globe.
By 2020, NASH is projected to overtake hepatitis C as the leading cause of liver transplants in the U.S. The disease is poised to win that dubious honor because an alarming rise in obesity and type-2 diabetes—key risk factors for NASH—is coinciding with far better treatments for hepatitis C.
Despite NASH’s prevalence, its obscurity isn’t surprising: It doesn’t cause obvious symptoms in most people, there’s no simple test to detect it, and no drugs have been approved to treat it.
On supporting science journalism
If you're enjoying this article, consider supporting our award-winning journalism by subscribing. By purchasing a subscription you are helping to ensure the future of impactful stories about the discoveries and ideas shaping our world today.
Within the next five years, that could change. The patient population is already sizeable and, barring vast lifestyle changes, it will continue to grow. NASH drugs could bring in as much as $8 billion annually—a figure that is grabbing the attention of companies both big and small. Today, the field has a packed pipeline of drugs, mostly small molecules, that offer multiple approaches to tackling the three hallmarks of NASH: fat accumulation, inflammation, and fibrosis on the liver.
Reversing the course of the disease will take a combination of drugs, liver specialists believe. That scenario has prompted a flurry of deal-making around NASH in the past two years as players such as Allergan, Bristol-Myers Squibb, and Gilead Sciences build portfolios of complementary products.
But even with heavy interest from drug developers and a rapidly advancing pipeline, there’s reason for caution. The field has so far only seen data from mid-stage clinical trials—results that range from encouraging to confusing to disappointing. And until researchers come up with a simpler way to diagnose NASH and detect whether fibrosis is improving, designing clinical trials that give a clear “yes” or “no” about a drug’s efficacy will be tricky.
Hidden damage
“This is a silent process, much like high blood pressure or diabetes,” explains Manal Abdelmalek, a liver disease specialist at Duke University. But unlike high blood pressure or diabetes, which doctors can detect with cheap and easy tests during a routine check-up, NASH is difficult to diagnose. Most people with scarring on their liver don’t display symptoms, and right now there’s no straightforward biomarker that a routine blood panel would pick up. The only reliable measure of fibrosis is a liver biopsy.
Moreover, the disease progresses slowly—over years or even decades—and researchers have yet to figure out when someone with a fatty liver is at risk for developing the inflammation and fibrosis that define NASH.
That subtle, slow-moving process begins with the build-up of fat in the liver, a condition called nonalcoholic fatty liver disease, or NAFLD, because it is not driven by alcohol consumption. According to the U.S. Centers for Disease Control & Prevention, up to 20% of the American population has NAFLD, which occurs when fat makes up more than 5% of the liver.
For many people, a fatty liver will never become a real problem. As Abdelmalek notes, “If you have isolated fat, you may live and die with your fatty liver and never know it.” But a portion of that population—a number pegged at roughly 16 million people—will go on to develop NASH’s telltale inflammation and scarring.
Anywhere from 1 million to 3 million people with NASH will go on to develop cirrhosis, where scarring has stiffened the liver so much that it can no longer function properly. From there, the outcomes can be grim: liver failure, liver transplant, or liver cancer.
Right now, a doctor can only recommend lifestyle changes—better diet, more exercise, less alcohol—to stop or reverse damage to the liver, which has an amazing ability to regenerate healthy cells. Unfortunately, studies have shown again and again that people are unable to stick to a healthier regime, and liver specialists would like to be able to offer treatments. The need for drugs is made more urgent by the fact that obese, diabetic people are often low on the liver transplant list.
But the road to NASH therapeutics is riddled with potholes. “The epidemiology of the disease is not particularly well described,” says Mike Burgess, who is in charge of Bristol-Myers Squibb’s fibrosis pipeline. Researchers still don’t know the speed at which NAFLD progresses, why some people with a fatty liver develop inflammation and scarring, and if particular groups of people are more at risk for developing cirrhosis.
And although researchers have theories about what will work, some stemming from other fibrotic diseases, their ideas still need to play out in the clinic. “The challenge with fatty liver disease is that the targets are still not well characterized, the disease is very heterogeneous, the pathways are complex, and the animal models don’t characterize the human phenotype well,” Duke’s Abdelmalek says.
Leading the pack
Still, pharmaceutical companies are moving full steam ahead with a range of treatments for NASH. The most-watched drug in the pipeline is Intercept Pharmaceuticals’s obeticholic acid, which made headlines in 2014 when results from a Phase II study were published in the Lancet.
Funded and run by the National Institutes of Health, the so-called FLINT study was, at the time, the largest to use liver biopsies to compare fibrosis before and after a drug was given to people with NASH. The study also looked at a wide panel of markers in the blood to assess whether the drug was having an effect on the underlying drivers of the disease.
Of the 110 people given obeticholic acid, 45% saw a marked improvement in their “NAFLD score”—a measure of fat, inflammation, and swelling of liver cells—without their liver scarring getting worse. In contrast, only 21% of the 109 people given a placebo improved.
Those results allowed Intercept to start a Phase III study of obeticholic acid. Because of the NASH population’s heterogeneity, the trial will be huge: The goal is to enroll 2,500 people, the majority of whom have Stage 2 or Stage 3 liver fibrosis, meaning they have significant scarring but are not yet considered cirrhotic.
The launch of the study, which defines the patient improvements the U.S. Food & Drug Administration wants to see before it approves a drug, has been critical to researchers in the field. In working with FDA to come up with an acceptable trial design, Intercept laid out a blueprint for other companies to follow as they push their own NASH drugs into the clinic.
For diseases without approved drugs, “having clarity and plans for designing a Phase III program that can be done in a finite period of time at a typical cost is important,” notes Lloyd Klickstein, head of translational medicine for Novartis’s new indication discovery unit. “It doesn’t make sense to start a program if you can’t finish it.”
Industry confidence in the path to regulatory approval has contributed to the recent spate of licensing and acquisitions of NASH-related assets. Rohit Loomba, director of the University of California, San Diego’s NAFLD Translational Research Unit, who has designed many of the clinical studies of NASH treatments, noticed an almost immediate explosion in interest in the field after the FLINT trial results were published. “Suddenly we went from five to 15 companies overnight, and now we are at 50 companies,” he says.
Recent notable deals include Bristol-Myers Squibb’s option to purchase Promedior and Gilead’s acquisition of Nimbus Therapeutics’s family of allosteric inhibitors of acetyl-CoA carboxylase (ACC), an enzyme critical in fatty acid synthesis. And last month, Allergan made a splashy entrance into NASH by buying two companies in one day: Tobira Therapeutics and Akarna Therapeutics.
The price of entry for the acquirers has been high. Allergan, for example, agreed to pay up to $1.7 billion—19 times Tobira’s market value—to capture cenicriviroc, which blocks two immunomodulatory receptors, CCR2 and CCR5, and is poised for Phase III studies.
Gilead’s deal with Nimbus, which brought an ACC inhibitor that just began Phase II studies, was similarly rich. “We had four offers on the table for the ACC program,” says Nimbus Chief Executive Officer Don Nicholson. Gilead didn’t make the highest bid, he adds, but the company’s existing NASH pipeline and experience in navigating combination therapies made it the most attractive.
Backbone search
In addition to sealing NASH’s fate as a hot therapeutic area, the FLINT data helped make the farnesoid X nuclear receptor (FXR) the drug target du jour. In addition to Intercept’s obeticholic acid, FXR agonists from multiple companies—including Gilead, Novartis, and Enanta Pharmaceuticals—are already in early to mid-stage studies.
NASH drugs generally fall into two buckets: molecules that address the fat or inflammation that drive the disease and molecules that address the injury they cause, namely scarring and cell death.
FXR has become an attractive target because it has a hand in regulating multiple contributors to the complex disease: the synthesis and transport of bile acids, the breakdown of lipids in the liver and intestine, and the maintenance of glucose levels.
Obeticholic acid is an analogue of one of FXR’s natural ligands, the bile acid chenodeoxycholic acid. Hewing close to the bile acids made by our bodies gives obeticholic acid its activity but also carries liabilities: bile acids don’t just bind to and turn on one receptor, and that promiscuity opens up the possibility of side effects.
Indeed, two side effects have emerged in studies of obeticholic acid, which has already been approved to treat another kind of liver disease. Many people given obeticholic acid experienced pruritis, or itchiness, a side effect that most have been able to control with other drugs or by taking a break from obeticholic acid. More worrisome for a drug serving a patient population that tends to have other health issues was an increase in LDL, or “bad,” cholesterol.
Although the cholesterol can be lowered by pairing obeticholic acid with statins, competitors see an opening to synthesize non bile-acid compounds that are safer and more effective. Moreover, a second trial of obeticholic acid, involving Japanese people with NASH, did not show the efficacy seen in the FLINT study. Competitors think a more potent compound could improve the antifibrotic effect of FXR agonists.
“That molecule is far from ideal in many respects,” says John McHutchison, executive vice president of clinical research at Gilead, which has an FXR agonist in Phase II studies.
The obvious areas to improve upon are the potency and selectivity of FXR agonists. FXR is a straightforward target for medicinal chemists: Companies have easily developed potent compounds targeting other nuclear receptors, all of which have natural ligands.
For example, the latest compound to enter the clinic, Enanta’s EDP-305, is 20 times as potent as obeticholic acid. Enanta CEO Jay Luly says his company’s chemists have already come up with next-generation compounds that boast 10,000 times the binding affinity for FXR of the Intercept molecule.
Akarna was launched just 18 months ago, but by the time Allergan acquired the firm last month it had discovered a new class of FXR agonists with high selectivity for FXR. The firm’s lead molecule, AKN-083, is expected to enter the clinic in early 2017.
Intercept’s CEO, Mark Pruzanski, is well aware of the bull’s-eye planted on his company’s lead compound. He counters competitors’ claims about obeticholic acid’s potency and selectivity limitations by noting that a handful of non bile-acid FXR agonists have already failed in early clinical studies in other diseases. Intercept will not have the first set of data from its Phase III study until 2019.
Beyond FXR
Many companies are pursuing FXR agonists because they believe their antifibrotic effect, if sufficiently potent, could make them a cornerstone therapy in the treatment of NASH. But the drug pipeline is also full of drugs—many repurposed from other diseases—that work by different mechanisms.
Liver specialists agree that they will need multiple treatment options to serve a diverse population. “Different patients are likely getting to NASH by different routes, such as different genetic predispositions or environmental exposures,” says Brent Tetri of St. Louis University’s Liver Center. “I don’t think we’ll get that one blockbuster drug that works for everybody.”
With that in mind, the big players in NASH are assembling portfolios of drugs with hopes of becoming leaders in a potentially lucrative market.
When McHutchison, a liver specialist, came to Gilead from Duke in 2010, he helped map out a NASH strategy intended to address multiple symptoms and drivers of the disease—namely, fibrosis, inflammation, and glucose and lipid metabolism. “I thought that targeting all components that cause the disease was going to be far more successful than just focusing on one of them,” McHutchison says.
Six years later, Gilead has four different types of drugs in the clinic. In addition to its early-stage FXR agonist, the company has simtuzumab, a monoclonal antibody in Phase II studies that tries to stop fibrosis by inhibiting the protein LOXL2; GS-4997, a small molecule meant to reduce inflammation and fibrosis by blocking the protein kinase ASK1; and GS-0976, an allosteric inhibitor of ACC that prevents fatty acid synthesis.
Bristol-Myers Squibb has taken a different strategy over the past two years by building a broader antifibrosis portfolio through internal research and deals that include options to acquire Galecto Biotech and Promedior. It also collaborates with the California Institute for Biomedical Research.
The company’s thinking is that its fibrosis assets, though initially positioned for other diseases, could be relevant in NASH.
“One of the things we’re still not clear on as a community is to what extent fibrosis is generic,” BMS’s Burgess says. In other words, researchers still don’t know if a drug that addresses scarring in lung tissue could also address scarring in the liver. “We have reasons to believe that should be true,” he says, noting that BMS is now thinking about how Promedior’s treatment for idiopathic pulmonary fibrosis could be used for NASH.
Allergan last month became the newest entrant in the NASH sweepstakes, buying an entire pipeline in one fell swoop with its acquisitions of both Tobira and Akarna. “We are putting a big marker on this disease,” Allergan CEO Brent Saunders said in a conference call after the deals were announced.
The next trials
As the NASH pipeline becomes increasingly crowded, researchers are seeking better ways to measure the disease’s hallmark fibrosis. Currently, the degree of liver fibrosis can be confidently detected only with a biopsy, a procedure that patients in a clinical trial need to endure before and after treatment to assess a drug’s efficacy.
“We’re talking about sticking a big needle through your side, into your liver, and taking a tissue sample of your liver before and after” treatment, Intercept’s Pruzanski notes. For patients, biopsies are unpleasant and risky; for companies conducting the trials, biopsies are expensive and time consuming.
And a liver biopsy is an imperfect way to measure fibrosis. Liver scarring is not evenly distributed, meaning the level of fibrosis seen in a sample depends on where the needle is inserted. To account for that natural variability, clinical trials such as Intercept’s Phase III study of obeticholic acid need to be huge.
Without simple ways to reliably detect liver fat and fibrosis, the use of any drugs that make it to market could be limited. “Even if we have effective therapies for NASH, the reality is many patients will still come to us with cirrhosis or advanced fibrosis because it was never discovered,” Tetri, the liver specialist, says.
UCSD’s Loomba has, over the past 15 years, become the leader in assessing how imaging tools and other techniques can be used to diagnose and treat NASH. Among his many efforts, Loomba has studied the use of MRI to measure liver fat—a test he is now hoping to show can be replaced by cheaper ultrasound techniques—as well as ways to use imaging to study liver stiffness.
And researchers still need to work out how NASH drugs will be used in the real world. If the industry develops a drug that actually reverses the disease, the question will be, “Do you stay on it for a year or two and then stop? Or do you stay on it forever?” Gilead’s McHutchison asks. “We’ve been discussing this recently internally and would have to look at both options and design trials that address both.”
Opinions on the subject differ. Some involved are convinced that—barring a significant change in diet and exercise to prevent fat from continuing to accumulate in the liver—people will need to be treated chronically, much like with a diabetes drug. Intercept’s Pruzanski says the treatment approach will likely come down to how effective drugs are at sustainably reversing the course of the disease.
But with the right tools to measure the markers of NASH, some liver experts believe, it might be possible to treat for a finite period and then monitor for changes. UCSD’s Loomba, for example, is confident that doctors will eventually be able to use blood tests and imaging tools to understand how a patient is responding to a treatment, possibly allowing those with early-stage disease to be treated acutely rather than chronically.
In the end, everyone agrees that treating NASH is a work in progress—albeit rapid progress. “I’m learning new things every two months,” Loomba says. “I say to myself, ‘Oh, I was so foolish I used to think that way.’ ”
This article is reproduced with permission from Chemical & Engineering News (© American Chemical Society). The article was first published on October 3, 2016.