I have died many times over. Every night when I lay down my weary self to rest, my consciousness is extinguished. I experience nothing until I wake up inside my sleeping body—in a dream disconnected from the external world. Or later consciousness resurfaces in the morning on my return to the wakening world.
Daily life contains many such experiences. In my childhood, I had an appendectomy and was anesthetized—my consciousness was switched off and, following the surgery, was restored. A fading memory from my teenage years places me in the back seat of a Renault that is driving down a tree-lined avenue in North Africa. Suddenly, the scenery changes abruptly. I’m on the same street, seeing things now from the ground up. The car had hit a tree, ejecting me onto the cobblestones, and I lost consciousness.
Many readers will have had similar recollections of consciousness lost and regained. We are used to the diurnal cycle of waking, sleeping and dreaming. But that experience is not the same for everyone. For some patients with brain trauma, consciousness flees for days, weeks or longer.
On supporting science journalism
If you're enjoying this article, consider supporting our award-winning journalism by subscribing. By purchasing a subscription you are helping to ensure the future of impactful stories about the discoveries and ideas shaping our world today.
In practice, a clinician may have difficulty establishing whether someone is quietly sleeping, anesthetized or severely brain-injured. Is a person lying with eyes open experiencing anything, no matter the content, or has the conscious mind fled the body and left no one at home?
Ideally, a technology could be devised to serve as a form of consciousness meter to answer these questions. At first, the idea of the equivalent of a blood pressure cuff for consciousness might seem absurd. But the development of several new technologies has raised real prospects for detectors that meet the criteria for consciousness meters—devices useful in medical or research settings to determine whether a person is experiencing anything at all. This ability to detect consciousness could also help physicians and family members make critical decisions, such as withdrawal of life-sustaining therapy, for tens of thousands of uncommunicative patients.
Recording Brain Waves
Contemplating the possibility of a consciousness meter requires consideration of the internal dynamics of our mental life, activity that waxes and wanes within fractions of a second, dictating the measuring of those fluctuating brain signals at a similar timescale. The most important physiological tool to infer consciousness from probing the brain has been, and continues to be, the electroencephalogram (EEG).
The EEG was developed by German psychiatrist Hans Berger, whose lifelong quest was to uncover the link between objective brain activity and subjective phenomena. He recorded the first ever brain waves of a patient in 1924 but, filled with doubt, did not publish his findings until 1929. The rest is history, as the EEG became the foundational tool of an entire field of medicine called clinical neurophysiology, although Berger was never accorded any significant recognition in Nazi Germany and hanged himself in 1941, despite being nominated for the Nobel Prize several times.
There are, of course, other ways to record brain activity besides the venerable EEG. The most common tools measure the dynamics of blood flowing inside the brain with magnetic scanners or track the magnetic field around the brain with magnetoencephalography (MEG). Yet these instruments, as well as more recent techniques such as near-infrared spectroscopy, come with methodological and practical issues that preclude their routine clinical use for the time being.
The EEG measures the tiny voltage fluctuations (10 to 100 microvolts) generated by electrical activity across the neocortex, the brain’s outer surface, which is responsible for perception, action, memory and thought. The main actors whose collective electrical activity is thought to be responsible for the EEG signals, via a mechanism known as volume conduction, are cortical pyramidal neurons, named for their tetrahedral shape. Contributions from deeper structures, such as the thalamus, have to be inferred indirectly via their action on cortical cells. The technology relies on electrodes placed directly on the scalp—that is, without the need for invasive surgery to penetrate the skull. With the move toward high-density EEG setups—with up to 256 electrodes—maps showing the distribution of electrical activity across the brain have become commonplace.
Still, placing the electrodes with their wet, conductive gel onto the scrubbed skin of the head is cumbersome, time-consuming, and prone to errors if the electrodes move, all of which limits the technology. With today’s more sensitive dry electrodes, the EEG is morphing from a clinical tool into a consumer device that can be used for biofeedback—allowing athletes or do-it-yourself “brain hackers” to focus their thoughts or insomniacs to track, deepen and extend their naturally occurring sleep.
From the late 1940s onward, detection of an “activated EEG” signal was the surest sign of a conscious subject. This state is characterized by low-voltage, rapid up-and-down fluctuating waves that are desynchronized rather than in lockstep across the skull. In general, as the EEG shifts to lower frequencies, consciousness is less likely to be present. Yet there are enough exceptions to this rule that it cannot serve as a general basis to diagnose absence or presence of consciousness in a given individual. Thus, scientists and clinicians alike have cast about for more reliable measures and have now found one based on a fundamental property of any conscious experience.
Into the Netherworld
Before we come to that, we should consider why clinicians care about detecting consciousness in two distinct groups of patients (pediatric patients represent a different challenge that will not be addressed here). The first consists of adults with severe disorders of consciousness following traumatic brain injury caused by gunshots, falls, accidents, and so on, infections of the brain (encephalitis) or its surrounding protective layers (meningitis), stroke, or drug or alcohol intoxication. After surviving the initial insult, patients are stable but disabled and bedridden, unable to speak or signal their thoughts and intentions. With proper nursing care to avoid bedsores and infections, these patients can live for years.
In this first group, clinicians distinguish several subcategories. Patients in a vegetative state, which is better described by the less pejorative term “unresponsive wakefulness syndrome” (UWS), cycle in and out of sleep. Yet setting up a bedside communication channel—“if you hear me, squeeze my hand or move your eyes”—meets with failure. UWS patients do swallow, yawn, and open and move their eyes or head but not in a seemingly intentional manner. No willed actions are left—only brain stem reflexes, activity that controls basic processes such as breathing, sleep-wake transitions, heart rate, eye movements and pupillary responses. Terri Schiavo is a name many remember, a patient in Florida who, following cardiac arrest, was resuscitated and lingered for 15 years in UWS until her medically induced death in 2005. UWS patients are a modern phenomenon depending for their survival on the infrastructure of 911, emergency helicopters and advanced medical care. There are more than 10,000 such individuals in the U.S. alone, living in hospices or nursing homes or at home.
Whereas behavioral evidence is compatible with the notion that UWS patients do not experience anything, it is important to recall that “absence of evidence is not evidence of absence” and to give the patients the benefit of doubt. There is a diagnostic gray zone into which UWS patients fall as to the question of whether their injured brains are capable of experiencing pain, distress, anxiety, isolation, quiet resignation, a full-blown stream of thought—or perhaps just nothing. Some studies have suggested that 20 percent of UWS patients are conscious and are therefore misdiagnosed. To family and friends who may care for their loved one for years, knowing whether anybody is mentally there can make a dramatic difference.
The situation is less ambiguous for minimally conscious state (MCS) patients. Unable to speak, they can signal but often only in a sparse, minimal and erratic fashion, smiling or crying in appropriate emotional situations, vocalizing or gesturing on occasion, or tracking salient objects with their eyes. Here the assumption is that these patients do experience something, however minimal, at least some of the time.
Credit: Amanda Montañez; Source: “Stratification of Unresponsive Patients by an Independently Validated Index of Brain Complexity,” by Silvia Casarotto et al., in Annals of Neurology, Vol. 80, No. 5; November 2016
The need to monitor consciousness also arises in a second, totally different set of patients who have a normally functioning brain—people who undergo invasive surgery for the usual host of ills, such as injuries, removal of a cancerous growth, or repair of knees, hips and other body parts. Anesthesia eliminates pain and other conscious experiences, prevents mobility and stabilizes the autonomic nervous system, which controls breathing and other functions, for hours at a time.
Patients “go under” with the expectation that they will not wake up during surgery and that they will not have to contend with traumatic memories of intraoperative experiences that could haunt them for the rest of their lives. Unfortunately, this goal is not always met. Intraoperative recall, or “awareness under anesthesia,” can occur in a small number of operations, estimated to be in the one-per-1,000 range, in particular when patients are paralyzed during a procedure by an anesthesiologist to facilitate intubation and prevent gross muscle movements. Given that millions of Americans undergo surgical-level anesthesia every year, this tiny fraction translates into thousands of awakenings under anesthesia.
Existing EEG measures monitor depth of anesthesia during an operation. Yet none of the vast diversity of anesthetic agents work in a consistent manner across all patients, who range from neonates to birthing mothers, the very elderly or the very sick. What is needed is a tool that can reliably track the presence of consciousness in individual subjects across a large spectrum of normal and pathological conditions under both acute (anesthesia) and chronic conditions (the plight of neurologically impaired patients).
The Nature of Conscious Experience
To detect consciousness, it is necessary to consider two essential characters of any subjective experience, no matter how mundane or exalted. First, by definition, any experience is different from all other experiences. It is specific to the moment and place in which it occurs. Each one is highly informative—take the unique visual richness associated with a mountain hike in the Rockies or another in the Cascade Range. Now combine these recollections with other sensory modalities, such as sounds and smells, emotions and memories. Each one is distinct in its own way. The second point is that each experience is seamless, integrated and holistic. You cannot separate the iconic percept of black smoke arising from the burning Twin Towers on a backdrop of blue sky into a half experience of the North Tower and another half experience of the South Tower.
The current most promising scientific theory of consciousness, which encompasses both of these ideas, is Integrated Information Theory (IIT). Devised by Giulio Tononi, a psychiatrist and neuroscientist at the University of Wisconsin–Madison, IIT emphasizes the differentiated and integrated aspect of any subjective experience and postulates that the mechanism supporting conscious experience in the human brain’s neocortex must likewise incorporate these two attributes. To probe the extent to which these mechanisms are intact, Tononi, together with a team that included neurologist and neuroscientist Marcello Massimini, now at the University of Milan in Italy, devised an EEG-based method back in the early 2000s. It provides a very crude approximation of IIT’s formal calculus. The team verified its basic soundness by correctly discriminating between when six healthy volunteers were conscious but quietly resting with eyes closed and when they were deeply asleep and therefore unconscious.
The brain of a deep sleeper acts like a stunted, badly tuned bell. Whereas the initial amplitude of the EEG is larger than when the subject is awake, its duration is much shorter, and it does not reverberate across the cortex to connected regions. While neurons remain active in deep sleep, as evidenced by the strong response in a local brain region, integration has broken down. Little of the electrical activity found in an awake brain is present.
Although distinguishing the brain’s response during a restful state from its response while sleeping may seem trivial, the method can be extended to the more difficult task of discriminating among a variety of brain states. Indeed, in subsequent years, Tononi, Massimini and 17 additional doctors and brain scientists tested the procedure in many more subjects. A paper summarizing this landmark study was published in 2016 in the peer-reviewed literature.
The method perturbs the brain by sending one or two pulses of magnetic energy via an enclosed coil of wire held against the scalp, a method called transcranial magnetic stimulation, or TMS. This technique induces a brief electric current in the underlying cortical neurons, which, in turn, engage other neurons in a cascade that reverberates inside the head before the electrical surge dies out in a fraction of a second. Think of the brain as a large church bell and the TMS device as the clapper. Once struck, a well-cast bell will ring at its characteristic pitch for a considerable time, as does the brain. Its electrical activity is monitored by a high-density EEG cap worn by the patient. The EEG is averaged and displayed during the course of 200 TMS pulses, as if it were a movie unfolding in time.
In an awake brain, with intact connectivity, this monitoring of different areas in response to the probe shows a highly complex pattern over much of the cortex, activity that is neither totally predictable nor completely random—and is emblematic of what is meant by “complex.”
The researchers estimate its complexity, the extent to which this response differs across the cortex and across time, using a mathematical measure capturing its diversity. The technique itself is borrowed from computer science and is the basis of the popular “zip” compression algorithm for reducing the storage demand of images or movies, which is why the entire procedure of measuring consciousness is known in the trade as zap and zip. Ultimately each person’s EEG response is mapped onto a single number, the perturbational complexity index, or PCI. If the brain does not react to the magnetic response—say, because the cortical activity is suppressed or only wiggles minimally—PCI will be close to zero, whereas maximal complexity yields a PCI of one. The larger the PCI, the more diverse the brain’s response to the magnetic pulse.
Zap and Zip in Patients
The logic of the 2016 study, which involved patients from specialized clinics in Belgium and Italy, is straightforward. In a first step, zap and zip is applied to a control population to infer a cutoff value—tagged PCI*—above which consciousness is thought to be present. In every case in which consciousness can be reliably established in any one subject, the person’s PCI values should be greater than PCI*, and in every case in which the subject is unconscious, PCI values should be below this threshold. This procedure establishes PCI* as a critical threshold—the minimum measure of complex brain activity—supporting consciousness. Then, in a second step, this threshold is used to infer whether consciousness is present in patients living in the gray zone, where more conventional measurements are insufficient.
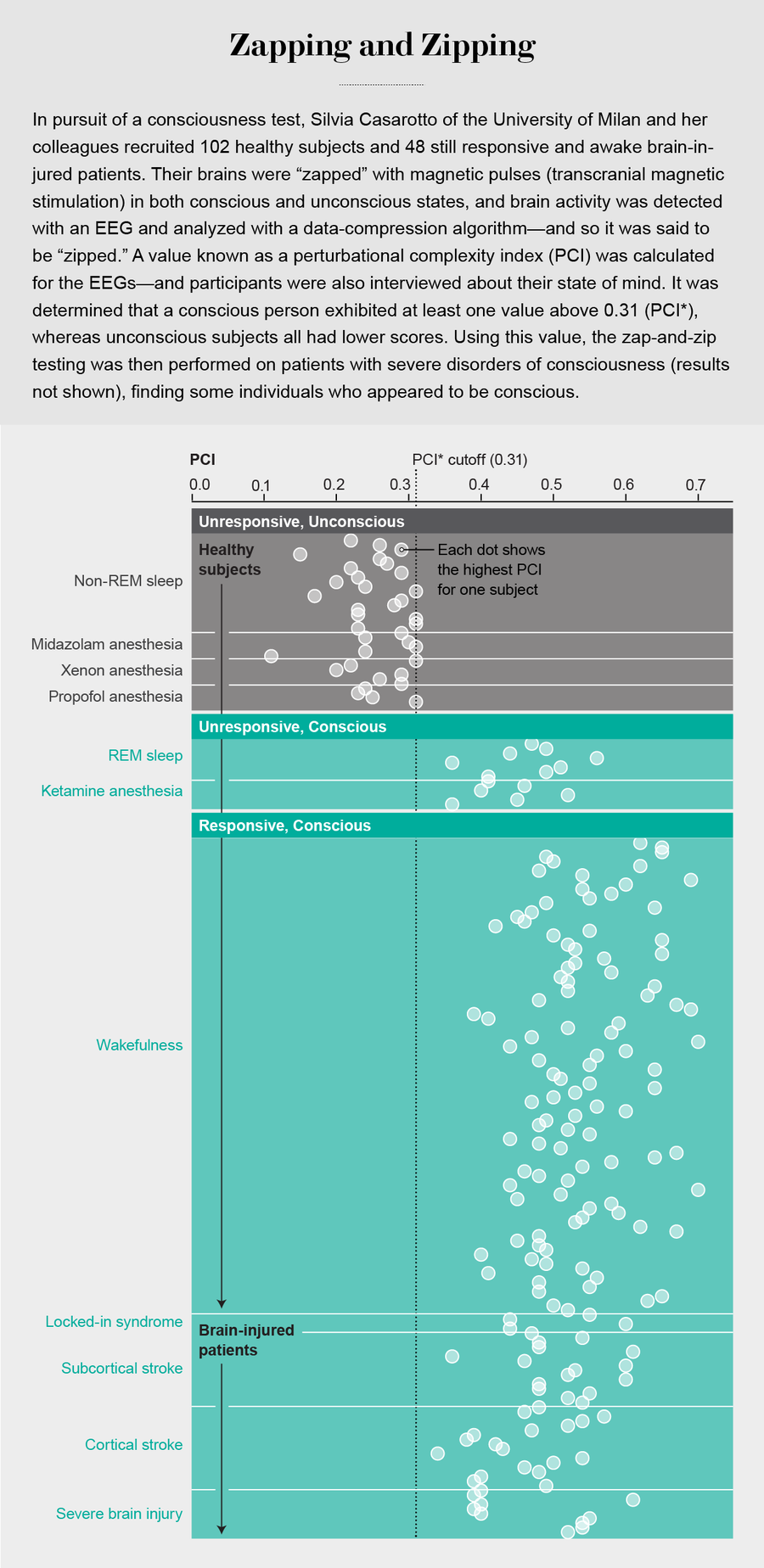
In the study, the benchmark population used to calibrate the procedure encompassed two groups. One consisted of 102 volunteers with no known brain impairment who experienced various conscious or unconscious states: quietly awake with eyes closed or dreaming during REM sleep (the latter is also a conscious state the researchers assessed by randomly awakening the sleepers during REM sleep and only including their EEGs in the final results if they reported any dream experience immediately prior to awakening). The EEGs were also assessed under anesthesia using ketamine, a pharmacological agent that disconnects and dissociates the mind from the external world but does not extinguish consciousness. (At a lower dose, ketamine is abused as a hallucinogenic drug, known as vitamin K.) The unconscious conditions for which EEG was measured during the study were deep sleep (reporting no experiences immediately prior to being awakened) and surgical-level anesthesia using three different agents (midazolam, xenon and propofol). The study also included 48 brain-injured but responsive and awake patients who were assessed while awake as controls.
The investigators found that consciousness could be inferred with complete accuracy in every single subject using the same PCI* value of 0.31. That is, in every one of the 540 conditions tested across the 150 subjects, if the electrical response was at or below this threshold, the subject was unconscious. If above PCI*, the subject was conscious. Everyone in the study, whether an uninjured volunteer or a brain-injured patient, received a correct classification. This achievement is remarkable given the variability in gender, age, brain locations where the TMS pulses were applied, and medical and behavioral conditions in the study cohort.
The team then applied zap and zip with this threshold value (of 0.31) to a distinct set of patients with severe disorders of consciousness—those either in a minimally conscious state or in an unresponsive wakeful one. In the MCS group, consisting of patients with at least some signs of behavior beyond reflexive functions such as breathing, the method correctly assigned consciousness to 36 of 38 patients, misdiagnosing the other two as unconscious. Of the 43 UWS patients, in which communication failed, 34 had a brain response whose complexity was less than that of anyone of the benchmark population when conscious, an expected result. That is, the complexity of their EEG responses was comparable to that of the benchmark group when not detecting consciousness.
Much more troubling, however, were the other nine patients who responded to the TMS pulse with a complex pattern of electrical activity that lies above the threshold. That is, the perturbational complexity of their brains’ responses was as high as in many conscious benchmark controls. These patients with high-complexity cortical responses may experience something yet are unable to communicate with the world and their loved ones.
As any successful experiment does, this one is leading to additional clinical studies. How can the zap-and-zip method be improved to achieve 100 percent accuracy in minimally conscious patients? Could other groups of patients, such as those with catatonia or late-stage dementia, infants, or young children, also be tested? Another question is whether other physiological or behavioral measures can be developed to corroborate the inference that some UWS patients are conscious. Can the method be turned into a prognostic tool, inferring to what extent UWS patients are on the road to recovery? Those questions need to be tackled moving forward. But in the interim, let us celebrate a milestone in untangling the ancient mind-body problem.

