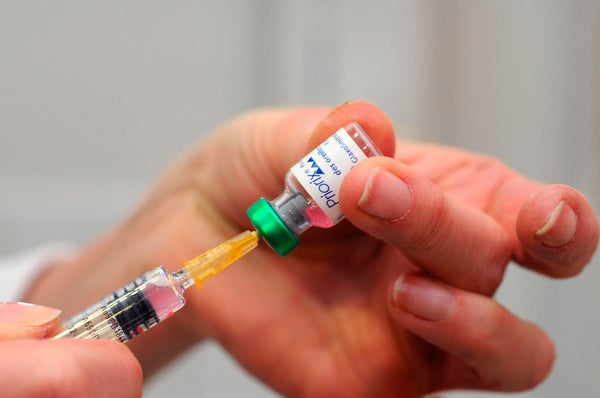
Passage of the Senate’s health care bill, as proposed, would risk eroding national health in one little-discussed way, according to medical experts: It would eliminate cash that pays for vaccines to protect the most vulnerable among us from diseases like mumps, measles or the flu.
Former Pres. Barack Obama’s Affordable Care Act (ACA) currently requires new health insurance plans to cover federally recommended vaccines for adults and children, without making patients share the costs through co-pays or deductibles—a “first dollar” coverage mandate meant to help Americans overcome the financial obstacle that had prevented some from obtaining important vaccinations. The bill also more broadly requires essential health services like vaccines to be covered by health insurers. Yet under the Senate proposal states could redefine what constitutes an essential benefit and can decide not to require coverage for certain preventive care—such as vaccines.
Without robust vaccine coverage, people may forgo immunizations as they did before ACA passed, says Amy Pisani, executive director of Every Child By Two, a nonprofit organization committed to reducing the burden of vaccine preventable disease.
On supporting science journalism
If you're enjoying this article, consider supporting our award-winning journalism by subscribing. By purchasing a subscription you are helping to ensure the future of impactful stories about the discoveries and ideas shaping our world today.
Initial data indicates the ACA vaccine coverage has already been helping more Americans get vaccinated and stay healthy: One study reported at the Pediatric Academic Societies annual meeting in 2016 showed that it led to higher vaccination completion rates for full diphtheria/tetanus/acellular pertussis (whooping cough), or DTaP, immunizations for young children. The greatest gains, they reported, were among children in families living at less than 200 percent of the federal poverty level. They had a 5.5 percent increase in on-time vaccination rates for the final dose of the vaccine, the authors wrote. Proponents of Republican-led health care reform, however, maintain the proposed changes would give states the flexibility to make their own decisions about how and when to support health within their borders.

An Obamacare logo is shown on the door of the UniVista Insurance agency in Miami, Florida on January 10, 2017. Credit: Rhona Wise Getty Images
If enough people stop getting inoculated against diseases such as measles, mumps or whooping cough, it could be disastrous for individuals and families, Pisani notes. For example, when large numbers of people get flu shots it creates herd immunity, which keeps everyone safer. It also helps protect populations for whom certain shots are too risky or ineffective (such as the elderly or those with compromised immune systems) by reducing their chances of encountering someone who is ill.
A rollback of vaccine funding—coupled with the Senate bill’s proposed demolition of Medicaid expansion—would make it more difficult for groups including the working poor to get vaccinations or other preventative care. And lower vaccine coverage would not be the only significant blow to public health, says Georges Benjamin, executive director of the American Public Health Association. The Senate bill would also zero out the Prevention and Public Health Fund (PPHF), which helps finance childhood vaccinations in addition to emergency preparedness and response. That fund pays for about 12 percent of the U.S. Centers for Disease Control and Prevention budget, Benjamin points out. “If people lose health care coverage, fewer people will be protected by vaccines that prevent cancer, pneumonia, and other painful and deadly conditions,” says Tom Frieden, CDC director under Obama. Then, if the CDC budget is slashed and the prevention fund eliminated “there will be further erosion of our country’s first line of defense against infections,” he says, noting that the prevention fund includes more than $300 million for vaccines.
If those cuts occur, Benjamin says, “we are less likely to find infectious disease early because uninsured or underinsured people go to the doctor later if not adequately insured—so sick people that are contagious are more likely to spread serious disease before detection.” Cutting the roughly $1-billion PPHF would also make it difficult to address the next big public health threat, says Peter Hotez, dean of the National School of Tropical Medicine at Baylor College of Medicine. Against the backdrop of Ebola, Zika and yellow fever as recent global health issues, he warns, it would be unwise to take such chances.