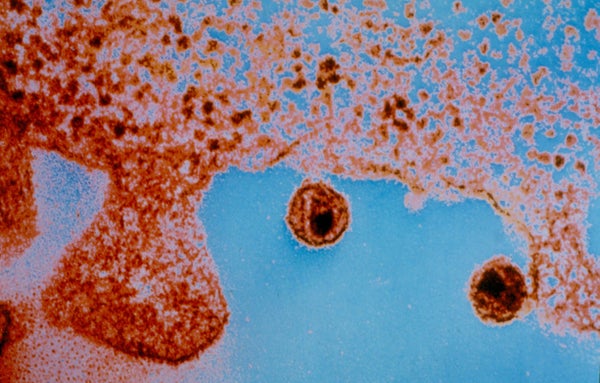
Thirty-six years ago, we were, like today, in the midst of a new and still somewhat mysterious global pandemic.In the U.S. alone, more than one million people were infected with HIV, and 12,000 had already died of AIDS. At the time, we were just beginning to understand how the virus worked. But that didn’t stop some leaders from making wildly optimistic claims about an AIDS vaccine being delivered within two years.
Now, with COVID-19, we are in a remarkably similar spot: 2.7 million people have been infected across the U.S., and 128,000 have died of the disease. Despite our limited understanding of how the novel coronavirus works and what it does to the human body, many are putting what I consider a disproportionate amount of faith in the possibility of a COVID-19 vaccine by 2021. My feelings today echo my feelings a third of a century ago: yes, a vaccine may be possible, but it is by no means a certainty.
Every deadly virus tells a story. As each chapter unfolds, we learn more about the possibility of developing a vaccine. The poliovirus, for example, told us early on that a vaccine would be possible. When that virus enters the body, it responds by making antibodies that can clear the pathogen entirely. It’s a hit-and-run: The virus hits you hard, then runs away for good. Once you have the antibodies, it can’t cause you harm again.
On supporting science journalism
If you're enjoying this article, consider supporting our award-winning journalism by subscribing. By purchasing a subscription you are helping to ensure the future of impactful stories about the discoveries and ideas shaping our world today.
With HIV, the virus told us the road to a vaccine would be long and challenging. As the outbreak unfolded, we began tracking antibody levels and T cell counts of those infected. The high levels of both showed that patients were mounting incredibly active immune responses, more forceful than anything we’d seen for any other disease. But even working at its highest capacity, the body’s immune system was never strong enough to clear the virus. Unlike a hit-and-run such as polio, HIV was a “catch it and keep it” virus—once you were infected, the pathogen stayed in your body until it destroyed your immune system and you died. While that situation didn’t mean a vaccine would be impossible, it certainly meant developing one wouldn’t be easy.
SARS-CoV-2 has echoes of both HIV and polio. We know from nearly 60 years of observing coronaviruses that a body’s immune system can clear the virus. But a coronavirus is a tricky thing. The virus distorts the immune system so that even after you clear it, the pathogen can reenter your system and cause illness again. It is not a hit-and-run or a catch and keep but a “get it and forget it” virus that is able to infect the same person multiple times.
For those who are listening, SARS-CoV-2 is telling us the path to a vaccine is going to be filled with obstacles. While some people with COVID-19 make neutralizing antibodies that can clear the virus, not everybody does. So whether a vaccine will stimulate neutralizing antibodies in everyone is still unknown. Also unclear is how long those antibodies can protect someone from infection.
Another challenge regards one of the ways SARS-CoV-2 enters the body: through the nasal mucosa. No COVID-19 vaccine currently in development has shown an ability to prevent infection through the nose. In nonhuman primates, some vaccines can prevent the disease from spreading to the lungs. But those studies don’t tell us much about how the same drugs will work in humans, because the disease in our species is very different from what it is in monkeys, who don’t become noticeably ill.
A more serious obstacle is the potential safety of a vaccine. Many vaccines include powerful adjuvants that are meant to inflame the body’s immune system, making the vaccine itself work better. The adjuvants in some vaccines currently being tested have led to serious side effects among young and healthy patients, including at least one who landed in urgent care because of extremely high fever and who experienced fainting as well. If that’s what a vaccine does to the young, imagine then the side effects for the old and infirm, who are the ones most in need of a viable drug.
These are significant challenges for any vaccine developer and should give us pause before believing too readily in a safe and effective vaccine by 2021. The good news, though, is that even without a vaccine, we are not without hope. Other medical solutions may prove just as effective at breaking the chains of transmission. Coronaviruses happen to be a target-rich environment for other types of drugs that can prevent viruses from multiplying. For other viral diseases, such as HIV/AIDS, hepatitis C, and herpes simplex virus types 1 and 2, antiviral drugs can both treat patients who are ill and prevent others from becoming infected. Thanks to these antivirals, new HIV infections in the U.S. have long been on a steady decline, and a positive HIV diagnosis is no longer a death sentence.
Antivirals have two common targets: polymerases, the enzymes a virus needs to copy its genome, and proteases, those needed to cut larger proteins into smaller, functional fragments. SARS-CoV-2 requires an active protease to copy itself. A couple of months ago a group of scientistsannounced their discovery of a new drug candidate that inhibits that protease. In test-tube experiments, they found the chemical could bind to the protease and prevent replication. And early results in dogs and mice suggest that the drug is both effective and nontoxic.
Though there is still much to be done before safety and efficacy in humans can be proved, the beauty of antivirals is that effectiveness can be determined much more easily than with a vaccine. Within a few days, you know your answer: either the drugs reduce the viral load in a patient, or they don’t. And you don’t need many people to prove it. Our first effective treatment for HIV wasinitially proved in a group of just 36 patients: 18 people who were given the drug and 18 controls.
While I admit to lacking confidence in our ability to deliver a COVID-19 vaccine by 2021, I am convinced we will have antiviral drugs to prevent and treat SARS-CoV-2 infection by next year, if not sooner. And perhaps not only antivirals. In the June 12 issue of Science, researchers published important progress on another approach to treat and prevent SARS-CoV-2 infections. This approach used monoclonal antibodies that stick to the SARS spike protein and prevent it from binding to ACE2 receptors in our body. Here, too, success can be gauged much more quickly than with a vaccine.
My hunger for a vaccine is as strong as the next person’s. My experience, however, tells me that hope for a quick COVID-19 vaccine may prove as misplaced as our hope for a quick HIV vaccine 36 years ago. I don’t doubt that it is possible. But while we wait on a scientific breakthrough, we should not lose sight of the solutions that are more easily within our grasp.
Read more about the coronavirus outbreak from Scientific American here. And read coverage from our international network of magazines here.