Arsenic’s potent effect on humans has been known since at least the Roman Empire. For centuries, it was a popular poison for murderers because it can’t be seen, smelled or tasted in food or water. That made it difficult to detect.
As chemical detection methods improved, its use as a poison declined. But arsenic, a naturally occurring chemical element in the Earth’s crust, remains a threat to human health. Regular, long-term exposure increases the risk of chronic disorders such as cancer, diabetes and heart disease for millions of people around the world.
For people, contaminated drinking water is the major source of exposure to inorganic arsenic, the form of arsenic that’s of most concern and has been the focus of research and regulation. (Rice and other foods may contain some, too, but are considered a much smaller risk to public health. Seafood can contain another form of arsenic that is bound to other molecules and is not a major worry for human health.) Globally, some 140 million people regularly consume water with arsenic levels that exceed the World Health Organization and US Environmental Protection Agency standard of 10 parts per billion (ppb).
On supporting science journalism
If you're enjoying this article, consider supporting our award-winning journalism by subscribing. By purchasing a subscription you are helping to ensure the future of impactful stories about the discoveries and ideas shaping our world today.
Biologist Rebecca Fry has long been concerned about this mass exposure. In 2006, researchers working in Chile reported that fetuses and young children exposed to arsenic-polluted water had six times the risk of dying from lung cancer later in life. This made a big impression on Fry, then a researcher at MIT. She helped run a study of pregnant women and their babies in a former mining area south of Bangkok to dig deeper into the effects of arsenic on human cells and genes.

Biologist Rebecca Fry.
Credit: James Provost (CC BY-ND)
The Thailand project inspired Fry to start a similar study in Gómez Palacio, Mexico, when she set up her lab at the University of North Carolina at Chapel Hill in 2008. Her team continues to analyze samples collected from the study participants to understand the impact of arsenic on fetal development.
Today, Fry is developing strategies to reduce human exposure to arsenic as the director of the UNC Superfund Research Program, a large project funded by the National Institutes of Health. The problem has both global and domestic relevance—rural North Carolinians, for example, may be unknowingly sipping dangerous levels of arsenic if they get their water from private wells, Fry has found.
Fry spoke with Knowable Magazine about recent discoveries and emerging strategies for reducing arsenic’s threat to human health. This conversation has been edited for length and clarity.
How widespread is human exposure to arsenic?
The largest and most concentrated number of affected people live in the state of West Bengal, India, and in Bangladesh. Scientists found that almost 40 percent of well water samples in Bangladesh contained arsenic above 50 ppb and 5 percent above 500 ppb, levels way above the WHO and EPA standard. I think scientists often know about most places with regular exposure above 100 ppb because many affected people develop unique skin lesions. But we are likely unaware of many places with lower levels of arsenic.
Case in point: Millions of Americans—almost 3 million in North Carolina alone—obtain their drinking water from private wells. The US Geological Survey estimated that roughly 10 percent of these have arsenic levels above the WHO standard. In North Carolina, we found 1,400 such samples, with a maximum of 800 ppb. What makes this so worrisome is that many well owners are not aware that their water is unregulated and may contain arsenic. Testing and treating it is their own responsibility.
How does arsenic get into drinking water?
Minerals in rocks naturally release arsenic into the soil through weathering and erosion. From the soil, it may dissolve in groundwater. These geologic processes are the main reason for contaminated drinking water in most countries, including India, Bangladesh and the United States. Human activities, such as mining and geothermal heat generation, can accelerate the release of arsenic.
An example of a non-geologic origin is coal ash, a byproduct of coal burning that contains arsenic and other toxic substances. This was a concern for a North Carolina community we are working with, but our analysis suggested that the arsenic found in their wells was geologic in origin.
What happens to arsenic in the human body?
In humans and other mammals, the main enzyme that converts arsenic into other chemical compounds is arsenite methyltransferase. The enzyme operates mostly in the liver and produces monomethylated and dimethylated arsenic, which we call MMA and DMA. Both of these breakdown products are excreted in urine, along with unconverted arsenic, but each has different health risks. Most people’s urine contains more DMA than MMA. The exact proportions vary by demographic and genetic factors.
In our studies, we measure arsenic in urine as an indicator of recent exposure. Toenail levels reflect chronic exposure. We estimate prenatal exposure from the mother’s urine and also umbilical cord blood.
How does arsenic exposure affect human health?
It depends on the proportions of these breakdown products. People with high MMA levels in their urine have a greater risk of various cancers. The link is strongest for lung, bladder and skin cancer. However, people with high DMA levels in their urine have a greater risk of diabetes. It is difficult to estimate the magnitude of risk since each study is different. For example, estimates depend on arsenic levels in the region’s drinking water and how arsenic is processed in the participants’ bodies. These distinct health risks show that we have a lot to learn about how arsenic and its breakdown products affect different cells and tissues.
Since arsenic crosses the placenta, fetal health is another concern. Some studies have reported harmful effects of prenatal and childhood exposure on brain development. In our Mexico study, prenatal exposure was associated with lower birth weight. We know from other studies that this may increase the risk of high blood pressure, kidney disease and diabetes in adulthood.
Someone’s health risk actually depends on both arsenic exposure and genetics. The gene that encodes the main arsenic conversion enzyme is called AS3MT. It comes in several versions that make the enzyme more or less efficient. A faster conversion process means less MMA and more DMA in the urine.
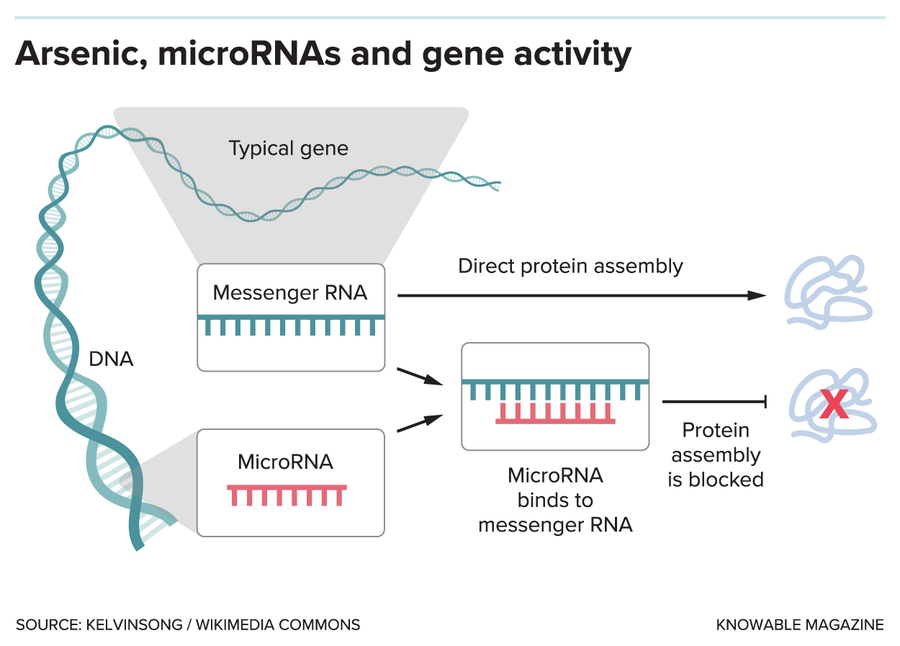
Arsenic’s effects on the body include altering how our genes behave. Genes are DNA sequences that contain information for making proteins, which control many processes in our body. Genes are expressed when they are copied into messenger RNA, which is then used to translate the genetic information into a functional protein. MicroRNAs (miRNAs) are tiny molecules made by DNA sequences that do not encode proteins. We have more than 2,000 different types of miRNA in our body. Each miRNA can bind to hundreds of messenger RNA molecules to block protein assembly. Arsenic can modify miRNA activity, and thus alter gene expression.
Interestingly, variation in the AS3MT gene may reflect past arsenic exposure in isolated populations. An example involves indigenous people in a small region of the Argentinian Andes. They have been drinking water with very high arsenic levels for thousands of years. This would normally mean increased rates of cancer and premature death.
But through natural selection, the population has adapted to living in this high-arsenic environment, which I find fascinating. A particular combination of variants in the AS3MT gene exists in almost 60 percent of the Andean women but is much less common in individuals elsewhere in the world. That combination probably explains much of the protection from arsenic’s toxic effects in this population.
What do we know about how arsenic causes disease?
The mechanisms are complex and vary by cell type and health outcome. A shared feature is that arsenic affects whether genes are expressed—as in, turned on or not—in key biological pathways.
In cancer, this could mean shutting down genes that repair DNA or that usually keep cells from growing into a tumor. In diabetes, it could mean disrupting genes that control the release of insulin in the pancreas or help other cells respond to insulin. These changes result from what are called epigenetic mechanisms, which alter gene expression without changing the DNA sequence itself.
One epigenetic mechanism involves microRNAs (miRNAs). People have more than 2,000 versions of these tiny molecules. Each miRNA can control the assembly of proteins encoded by hundreds of genes. This means they have a huge influence collectively. Studies have shown that arsenic can influence miRNA activity.
Another epigenetic mechanism is DNA methylation. Arsenic may influence whether methyl groups are added to specific DNA sequences. This can also reduce or prevent gene expression.
The KCNQ1 gene is an interesting example. Normally, the gene copies we inherit from both of our parents are expressed in our cells. But KCNQ1 is one of a few hundred genes where only one parental copy—the maternal or paternal one—may be expressed in some tissues. The other is turned off by methylation, either early in development or before conception.
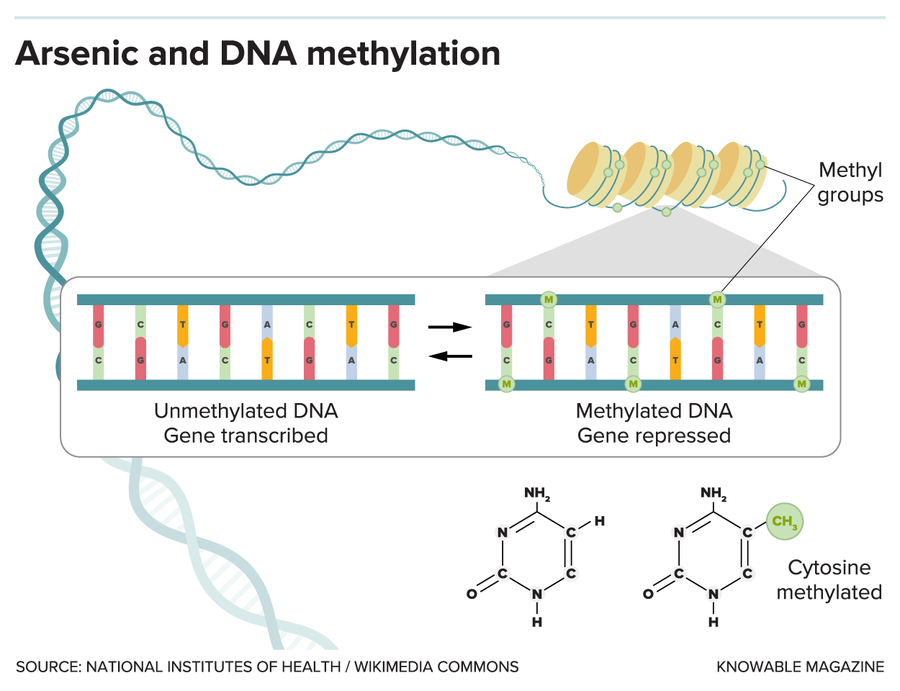
When active, a gene is transcribed and translated into a protein. But in a process called methylation, methyl groups (consisting of three hydrogen atoms bonded to a carbon atom) attach to a specific part of DNA (here, the nucleotide cytosine) and block the process. Scientists have shown that arsenic can affect gene activity by changing DNA methylation patterns.
In our Mexico study, prenatal arsenic exposure was associated with greater KCNQ1 methylation and reduced gene expression. Since KCNQ1 is important for embryonic development, this may help explain why arsenic is associated with lower birth weight. The same gene also influences insulin secretion in the pancreas. Thus, reduced gene expression may contribute to elevated blood glucose levels.
The possibility of very early KCNQ1 methylation in our human study prompted us to study the effect of preconception arsenic exposure in mice. My colleague Mirek Styblo and I found that exposing both parents to arsenic prior to conception caused early signs of diabetes in male offspring. If true for humans, the critical window of exposure would include the pre-pregnancy period. This would have huge implications for public health.
What can be done to reduce the dangers of arsenic?
In our Superfund Research Program, we are studying water treatment, nutritional and genetic interventions.
We found that low-cost water pitchers with a built-in filter reduced arsenic levels in water from private wells in the North Carolina communities we work with. However, the pitchers are slow to process large amounts of water. Environmental engineer Orlando Coronell and colleagues are developing household-scale systems that remain affordable for low-income populations. These could be integrated into faucets or installed under sinks.
Geologist Owen Duckworth and his team study how the depth of a well influences arsenic levels. This may lead to new well construction guidelines for reducing human exposure.
Nutritional factors can protect some individuals. For example, a 2006 clinical trial in Bangladesh showed that folic acid supplements reduced arsenic toxicity in adults whose diet is deficient in this key nutrient. The gut microbiome may help, too. We know that microbes in the mouse gut help convert almost all arsenic into DMA. More DMA means a lower cancer risk, so the microbes are beneficial in that sense. Kun Lu and his team are now studying if nutritional supplements can help human gut microbes reduce arsenic toxicity.
For our genetic research, we have a fantastic new tool developed by Mirek Styblo and Beverly Koller. For years, it was unclear what findings in mice mean for humans because mice break down arsenic very efficiently and have almost all DMA and no MMA in their urine. Styblo and Koller developed a new mouse strain that carries the human AS3MT gene, instead of the mouse version. Thus, the proportions of MMA and DMA in the mouse urine are almost identical to humans. This is a really big deal.
Praveen Sethupathy and colleagues are studying the effect of miRNAs. For example, one miRNA influenced by arsenic may affect the expression of KCNQ1 and other genes related to diabetes. A different miRNA may help convert arsenic by controlling AS3MT gene expression.
Genetic technology to reduce arsenic toxicity is, of course, more complex and expensive than water filters or dietary supplements. But doctors are already testing miRNA therapies for cancer. We hope that pursuing different strategies will ultimately help us identify solutions for exposure scenarios in North Carolina, Mexico and around the world.
This article originally appeared in Knowable Magazine, an independent journalistic endeavor from Annual Reviews. Sign up for the newsletter.
10.1146/knowable-030421-1

