The constant activity of nerve cells in the brain requires an ongoing supply of chemical energy. Nerve cells, also called neurons, get this energy by breaking down glucose in a long series of reactions. Most of the energy emerges from the last few reactions, which require oxygen. The brain receives both glucose and oxygen through the blood, which is pumped up to the brain by the heart via arteries in the neck. (The pulse of blood in one of these arteries, the carotid, can be felt by pressing your fingers gently on the side of your neck). The arteries branch out at the brain, carrying blood over and through the organ.
If the supply of oxygen to the brain cells is inadequate, the neurons cannot break down glucose completely. As a result, they do not obtain enough energy for their activities; also, the partial breakdown of glucose yields harmful waste products. These conditions not only prevent nerve cells from functioning normally, but can also injure and kill them. Further damage may occur later when the blood flow is restored (reperfusion injury) and free radicals form. Either way, this damage causes brain malfunction, which becomes evident as the signs and symptoms of a stroke.
Strokes are also called cerebrovascular accidents (CVAs) because they result from abnormalities in the heart or blood vessels, which cause either a reduction in blood flow to areas in the brain or hemorrhaging within the brain itself. The first are called ischemic strokes and the second, hemorrhagic strokes. Strokes are classified based on the timing of the signs and symptoms, which vary widely depending on where and how badly the brain is damaged. An ischemic stroke having signs and symptoms that disappear within 24 hours is called a transient ischemic attack (TIA). TIAs often reoccur because blood flow to the same brain area is reduced and may eventually be followed by more serious strokes. In a reversible ischemic neurological deficit (RIND), the signs and symptoms subside more slowly. In a progressive stroke, signs and symptoms develop gradually and get worse over time. If the signs and symptoms develop quickly and show very little or no improvement over time, a completed stroke has occurred.
On supporting science journalism
If you're enjoying this article, consider supporting our award-winning journalism by subscribing. By purchasing a subscription you are helping to ensure the future of impactful stories about the discoveries and ideas shaping our world today.
Most strokes result from atherosclerosis in arteries either within the brain or leading from the heart to the brain. Atherosclerosis leads to ischemic strokes by making arteries narrow, rough, stiff and weak. Narrowness reduces blood flow directly. Roughness reduces blood flow by causing the formation of blood clots (thrombi), which partially or completely block the vessel. Stiffness causes inadequate blood flow by preventing arteries from dilating when a region of the brain becomes more active and needs more oxygen or when blood pressure drops. Weakness in arteries can lead to reduced blood flow if the weak area bulges outward, forming an aneurysm. Though the region with the aneurysm is initially wider than normal, blood swirling in aneurysm can clot. As the clot enlarges, it can partially or completely block blood flow through the artery. Blood clots in arteries may break free of the vessel wall (embolize)--in which case flowing blood can push them into smaller arteries, where they block blood flow completely. Emboli formed by atherosclerotic plaque can also block arteries.
Atherosclerosis in arteries within the heart (coronary arteries) can also lead to an ischemic stroke by first reducing blood flow to the heart muscle. As the heart becomes weaker, blood flow to the brain decreases. If a heart attack occurs near the inner surface of the heart, it can cause a rough spot and clot formation inside the heart (mural thrombus). A heart weakened by atherosclerosis may also bulge outward (ventricular aneurysm), leading to clot formation. In either case, the clot from the heart may embolize into arteries leading to or through the brain. Ischemia then follows when the embolus blocks an artery. Sometimes many emboli develop, causing multiple strokes.
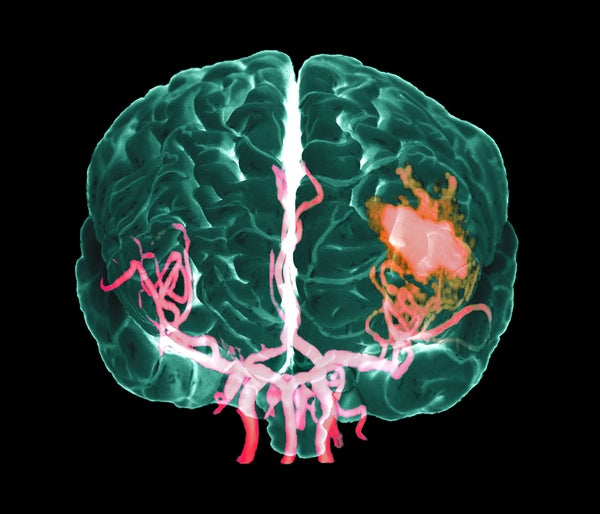
When atherosclerosis weakens an artery in the brain, the artery can burst, causing hemorrhaging within the brain. Congenital defects in brain arteries can also lead to hemorrhagic strokes. These types of strokes can develop in several ways. The area to which the artery was carrying blood becomes immediately ischemic. At the same time, the blood spurting from the artery can directly damage nerve cells. Indeed, hemoglobin leaking from dying red blood cells injures and kills neurons. Part of this injury is from free radicals formed in the presence of iron in the hemoglobin.
As the blood mass (hematoma) enlarges, it is the pressure on the surrounding neurons that injures and kills them. Also, the enlarging hematoma may push the brain toward one side of the skull. And as the brain shifts across the rough base of the skull, more injury occurs to brain cells and to nerves and vessels attached to the brain. Because the skull is a rigid container, further enlargement of the hematoma causes an increase in pressure throughout the skull, leading to more neuron injury and death. Inflammation develops in the injured areas, resulting in brain swelling, additional increases in intracranial pressure, and more neuron injury and death. As intracranial pressure rises, brain vessels become compressed, causing more ischemia throughout the brain. If the intracranial pressure becomes great enough, portions of the brain may be forced outward through skull openings, such as the foramen magnum at the base of the skull.
More on what causes strokes from Harold Adams, a professor of neurology at the University of Iowa:
The term stroke encompasses a number of blood vessel diseases of the brain. Approximately 20 percent of strokes are called hemorrhages, during which a blood vessel ruptures and bleeding occurs into or around the brain. The leading causes of hemorrhages are high blood pressure, disorders of bleeding (tendency to bleed) and abnormalities of the blood vessels, including blisters (aneurysms) or tangles of blood vessels (vascular malformation).
The other 80 percent of strokes are due to infarctions. In this situation, a blood vessel becomes blocked and blood can not reach an area of the brain. The area of the brain that does not receive adequate blood dies because of a lack of oxygen and other vital nutrients. Brain infarction is quite similar to an infarction in the heart, or heart attack. The most common cause of brain infarction is hardening of the arteries (atherosclerosis). However, a number of other conditions--including heart diseases, which produce clots that move to the brain (embolism), other diseases of blood vessels and disorders of blood that promote clotting--can also lead to brain infarction.
What happens to the body during a stroke? The brain is the most sophisticated computer ever created. Just as a computer can lose part of its programs due to a faulty chip or circuit, the brain too can lose functionality from stroke-induced damage. Because the brain controls the electronic circuits that make up the nervous system, damage to it presents problems such as loss of language, paralysis, loss of vision, poor balance and sensory loss. Clinical findings vary greatly depending on the location and extent of brain damage done by a stroke. A very severe stroke may even cause a loss of consciousness. As the name stroke implies, the event usually occurs suddenly. A patient can be literally struck down.