An outbreak of the Ebola virus in the northeastern Democratic Republic of the Congo (DRC) that has been raging since 2018 has officially ended. The World Health Organization (WHO) and the DRC government announced the end on 25 June—42 days after the last case—but it comes as a fresh Ebola outbreak spreads in the country’s northwest.
“We are extremely proud to have emerged victorious over an epidemic that has lasted a long time and caused a lot of damage to our population,” said Jean-Jacques Muyembe Tamfum, a co-discoverer of Ebola and the director of the National Institute for Biomedical Research in Kinshasa, at a press briefing.
After the outbreak was declared in August 2018, the virus infected at least 3,470 people, killing 66% of them. That makes it the world’s second-largest outbreak of the haemorrhagic disease, after the 2014–16 West Africa epidemic, which killed more than 11,000 people. Experts say that the northeastern epidemic—which mainly affected North Kivu and Ituri provinces—was one of the most complex health emergencies the world has ever seen, because it occurred in a region of the DRC plagued by 25 years of war and political instability. In the course of the outbreak, more than 70 Ebola patients and Ebola responders were injured in dozens of targeted attacks by armed groups. At least 11 were killed.
On supporting science journalism
If you're enjoying this article, consider supporting our award-winning journalism by subscribing. By purchasing a subscription you are helping to ensure the future of impactful stories about the discoveries and ideas shaping our world today.
Vaccine roll-out
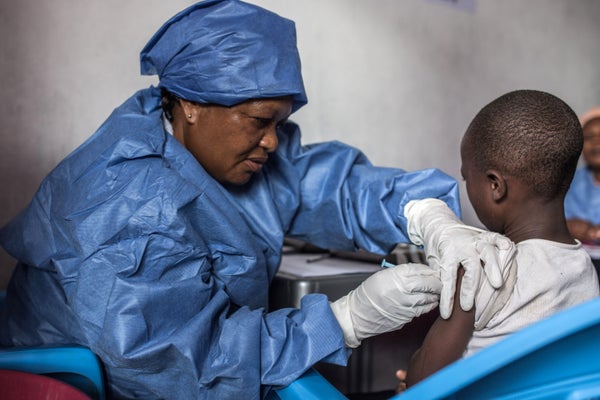
But the epidemic was marked by successes in vaccination and treatment. This was the first Ebola outbreak in which a vaccine for the virus was widely deployed. The vaccine, made by drug company Merck of Kenilworth, New Jersey, and first tested during West Africa epidemic, was given to more than 300,000 people who had been in close proximity to people with Ebola, and their contacts. More than 80% of people who were vaccinated didn’t end up with the disease, said Muyembe, and those who did had relatively mild cases.
A clinical trial conducted during the outbreak also found that two antibody-based drugs, called mAB114 and REGN-EB3, reduced deaths dramatically among people who were hospitalized soon after being infected. These were then given to all consenting patients in Ebola treatment centres in northeastern DRC.
Another key to success, said Muyembe, was local leadership. The rate of new infections in the region slowed after governors and mayors of cities hit hard by Ebola began pushing to stamp out the virus, and once local health workers had been trained and equipped to care for people, he said.
Coronavirus competes
Ebola responders now want to replicate these tools and strategies in Équateur, a province on the opposite side of the country, where 18 people have been reported to be infected with Ebola virus since an outbreak was declared there on 1 June.
But Ibrahima Socé Fall, the assistant director-general for emergency response at the WHO in Geneva, Switzerland, says the region is difficult to reach by car and motorcycle—complicating Ebola responders’ efforts. He is worried because Équateur’s health system is inadequate, and the population is extremely poor and moves around a lot. People frequently travel for trade to and from Mbandaka, a city of about one million people, to cities in the neighbouring Republic of Congo and the Central African Republic. That raises the risk that they could take the virus with them and spread it further, he says.
And although some doctors and researchers who were assisting in the northeast have relocated to Équateur, many others are now involved in efforts to fight COVID-19. There have so far been at least 6,552 confirmed cases of the coronavirus in the country, and 149 deaths.
“I’m really proud of my colleagues and we had thought we might really celebrate when this ended,” says Socé Fall, who spent last year in northeastern DRC. “But many people are already deployed to COVID, and we’re so busy,” he says. “There’s no time to get together.”
This article is reproduced with permission and was first published on June 26 2020.