In 2023 thoracic surgeon Ankit Bharat was working at Northwestern Memorial Hospital when he was drafted to help a 33-year-old influenza patient who was on the verge of death. Bharat recalls that the man had developed a secondary infection from one of the “most dreaded bugs” in the hospital, Pseudomonas, and had been put on a ventilator. The patient’s lungs were filling with fluid and pus, his kidneys were failing, and his heart was barely working, Bharat says. “He was actively dying.”
Then the patient’s heart stopped. “We got him back—but it was very clear we had to do something right away,” Bharat says.
The man needed a double-lung transplant, but there was a problem: he was too sick for Bharat and his colleagues to attempt the operation. But Bharat knew that without a working set of lungs, the patient would die regardless. He had already been on a life-support system called extracorporeal membrane oxygenation (ECMO) to oxygenate his blood, but that treatment can’t sustain a patient without lungs in their body, Bharat says.
On supporting science journalism
If you're enjoying this article, consider supporting our award-winning journalism by subscribing. By purchasing a subscription you are helping to ensure the future of impactful stories about the discoveries and ideas shaping our world today.
So Bharat and his team worked up a plan: they would build “artificial lungs” that could help pump blood from the right side of the patient’s heart to the left side, oxygenate it and send it on to the rest of the body.
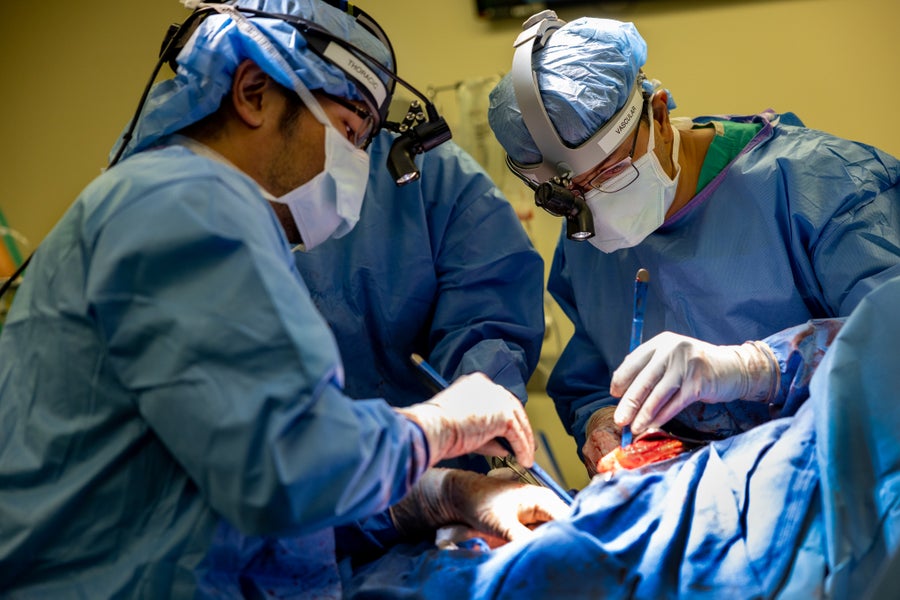
Chitaru Kurihara (left) and Ankit Bharat (right) operate on the patient, removing his damaged lungs and attaching the artificial lungs.
Northwestern Medicine
Bharat likens the novel system to adding a bridge to a highway: like interstate traffic, blood travels from the right side of the heart to the lungs, then to the left side of the heart and then throughout the body. With no lungs, the highway hits a dead end. Bharat’s artificial lungs literally bridged the gap—moving and oxygenating blood in place of the patient’s lungs, which were removed. And to prevent a “traffic jam” on that bridge, Bharat’s team also built an “exit” road for blood to return to the right side of the heart.
The system kept the patient alive for two days, effectively lungless, letting him begin to recover from the infection. “It was almost like a curse or something that just got lifted,” Bharat says. “And suddenly everything started to heal.”
The patient was placed on the lung transplant candidate list—and just hours later he had a donor. The team completed the transplant, and after some extra weeks of recovering in the hospital, the man was discharged, weak but alive.
Now, more than two years later, “he’s doing great, by the way,” Bharat says.
Systems similar to Bharat’s artificial lungs have been described by doctors before, says Matthew Hartwig, a professor of surgery at Duke University, who was not involved with the patient’s care. But Bharat’s method, he says, offers “a novel approach” to “the same problem that everyone is facing” in the field. The process is described in a paper published in the journal Med.
Bharat hopes his lung system can be used at other hospitals as a “nuclear option” to save patients who are critically ill. “We have described all the lessons that we’ve learned in that paper, how we came up with every single configuration, what is the rationale behind it, and anybody can replicate that,” he says. “There is nothing proprietary about this.”
He hopes it could ultimately mean there will be more success stories like that of the patient he helped save in 2023. “Even at the end of the day, if we save one extra life, we’ll be happy with that,” Bharat says.