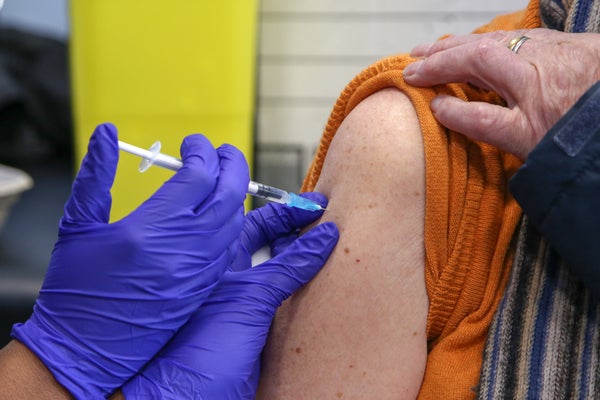
When physician Melanie Swift got her first COVID shot in January 2021, she felt as though the vaccines marked a turning point. “If we just get ’em in enough arms, we can beat this thing and not spread it,” says Swift, who co-chairs the COVID-19 Vaccine Allocation and Distribution Work Group at the Mayo Clinic.
Soon breakthrough infections came along, yet most hospitals seemed to hold up. Public health messaging began to pivot away from a focus on case numbers. “We started to say, ‘Okay, well, the important thing is people not dying and people not having to be at the hospital,’” Swift says.
Then, last September, data from Israel suggested that a third dose of mRNA vaccine could further enhance protection against severe disease in older adults. So the U.S. Centers for Disease Control and Prevention recommended booster shots—initially for people age 65 and older and other adults with a high risk of complications or exposure and eventually for everyone aged 12 years and older.
On supporting science journalism
If you're enjoying this article, consider supporting our award-winning journalism by subscribing. By purchasing a subscription you are helping to ensure the future of impactful stories about the discoveries and ideas shaping our world today.
The guidance shifted yet again in late March after the U.S. Food and Drug Administration authorized a second booster shot for immunocompromised people and for anyone age 50 and up.
Although the consensus remains that getting the initial full-series vaccination offers a clear benefit, scientists today disagree on the value of a fourth mRNA vaccine dose. Some say a second booster is essential for protecting highly vulnerable people—and that it should also be available to their families and other close contacts. Others note that the FDA’s decision about a fourth dose was based on limited evidence—primarily one study in Israel—and that the original two-shot series still provides durable protection against the most severe outcomes in adults with a healthy immune system.
For its part, guidance published on April 6 by the European Center for Disease Prevention and Control and the European Medicines Agency’s COVID-19 Emergency Task Force states that a fourth mRNA COVID vaccine dose can be given to adults age 80 and older but that it is too early to consider that booster for the general population.
In the short term, if the goal is to stop transmission when cases are rising and enhance society’s transition to more normal activities, boosters could conceivably help. “If you can quickly boost a bunch of people at the cusp of a surge, you might be able to flatten that curve,” Swift says. She notes, however, that boosters only temporarily slow the spread of infection.
Adding to the public’s risk calculation fatigue, many airlines lifted mask requirements last week after a federal judge ruled that a mask mandate on public transportation is unlawful. (The Department of Justice has since appealed that ruling.) “It feels like a mixed message to people to say, ‘Get your booster but stop wearing masks,’” Swift says. “It’s been such a quagmire.”
To explore how to evaluate the latest thinking on whether to get a second COVID-19 booster, Scientific American followed up with Swift and other experts in infectious diseases and immunology.
Who should get a second booster shot?
For those with elevated risk for severe illness because of age (50 years and up) or a weakened immune system—for example, people undergoing chemotherapy or organ transplant patients taking immunosuppressive drugs—“getting that second booster is really important,” says Brianne Barker, an immunologist at Drew University.
People who received the Johnson & Johnson (J&J) vaccine as both their primary and booster dose can also receive a second booster, according to updated CDC recommendations. A study published in March shows that J&J vaccine recipients produced weaker antibody responses than people who got the two-shot series of an mRNA vaccine.
Should eligible vaccinated individuals who recently recovered from an infection with the Omicron variant consider a booster?
Yes, but they probably should not do so right away. “There’s a real immunological argument to be made for letting that immune response mature and develop memory cells,” Swift says. “Two to three months after the infection would be a good window of time to get that booster.”
What other factors should people consider?
Local transmission rate: The CDC has an online tool that labels COVID risk by county as green (low), yellow (medium) or red (high)—determined by local factors such as hospital bed availability and the rate of new cases. As part of your own risk assessment, it is important to know “the landscape around you,” Swift says. “What kind of society are you going out into?”
Personal exposure risk and consequences of infection: Reported infection rates have hit a plateau in many parts of the U.S., Swift says. “If those start to tick up higher, I’d have a lower threshold to get [a second booster],” she adds. On the other hand, “if you’re someone who stays home and doesn’t go out to socialize, your risk may not be higher.”
Access to early treatments: Several oral medications can keep the disease from worsening if taken within the first five days of COVID symptom onset. In studies of high-risk adults, the FDA-authorized pills Paxlovid and molnupiravir reduced hospitalizations and deaths by 89 percent and 30 percent, respectively. “If you have health insurance and a primary care doctor who would prescribe those [pills], then maybe you’re okay,” Barker says. The federal Web site COVID.gov also directs consumers to tests, treatments and vaccination sites.
How much additional protection does a second booster shot provide?
So far most of the data comes from Israel, which in January began giving a fourth dose, or second booster, of the Pfizer COVID vaccine to people 60 years of age or older. In a retrospective analysis of health data on 1,252,331 eligible seniors, researchers found that rates of severe COVID were about 3.5-fold lower in the group that got a second booster, compared with individuals who had only received three Pfizer doses. Infection risk was halved during the first four weeks but then the benefit started to fade.
On the other hand, protection against severe illness did not wane among people with only three Pfizer doses during the study period.
Speaking to the uncertainty around the ultimate aim of boosters, other researchers point out that T cells, less studied but vital components of the immune response, could account for vaccines’ durable protection against severe COVID. T cells recognize and attack a broader range of viral components and thus “may be more adept at responding to infection with evolving viral variants than antibodies,” researchers write in a paper published in Science Immunology in March.
Most studies measure how well a COVID vaccine triggers the production of neutralizing antibodies, which glom onto the COVID-causing coronavirus SARS-CoV-2 and keep it from getting into cells. Once the virus starts infecting cells, however, neutralizing antibodies are not as useful. “You need a type of immune response that can actually deal with the infected cells, and that’s what T cells are for,” Barker says. “So even if you don’t have a good neutralizing antibody response, you could have a great response with some of these other immune cell types that can help you clear the infection. That might keep you from getting severe disease even if you are infected.”
The speculation derives from the fact that T cell responses are much harder to study. Whereas each person produces a similar set of antibodies against SARS-CoV-2, T cell responses vary. This is because of genetic differences between individuals and because of the manner in which T cells recognize antigens. “The test you would make to measure my specific T cell response would be a little different from the test to measure yours,” Barker says. Also, unlike antibody measurements, which can be done with just the liquid part of a blood sample, many measures of T cell immunity require the actual cells.
Will we need boosters on a regular basis?
This raises a bigger question about goals. Should COVID vaccines be designed and deployed primarily with the goal of preventing severe disease or also to prevent infection? “That’s not something we’ve ever really distinguished in the past when talking to the public,” Barker says.
Yet this distinction is crucial, and language matters. In an April 13 commentary in the New England Journal of Medicine, Paul Offit, director of the Vaccine Education Center at the Children’s Hospital of Philadelphia, expresses his disappointment with the labeling of SARS-CoV-2 infections in vaccinated individuals as “breakthroughs.” This term “implies failure” and “created unrealistic expectations,” he writes. “If we are to move from pandemic to endemic, at some point we are going to have to accept that vaccination or natural infection or a combination of the two will not offer long-term protection against mild illness.”
That said, some scientists foresee COVID boosters for years to come. “It’s pretty clear by now that SARS-CoV-2 is here to stay, and we’ll most definitely need some form of boosting moving forward,” says Benjamin Goldman-Israelow, an infectious disease physician-scientist at Yale University.
Some researchers are studying Omicron-specific vaccines, although results from mice have found only modest benefits from boosting against such newer variants, compared with using boosters designed around the original version of SARS-CoV-2.
Goldman-Israelow and others are developing a new type of COVID booster—a formulation that could be sprayed into the nose—that could further enrich the effects of conventional intramuscular vaccines by inducing antibody production and T cell responses in mucosal surfaces such as the nose, mouth and throat. In mice that received a vaccine against SARS-CoV-2, he and his colleagues at Yale showed in a preprint study that boosting with an intranasal vaccine against SARS-CoV (the coronavirus that caused the SARS outbreaks in 2002–2004) triggered high levels of antibodies to both coronaviruses.“So we think our strategy should be able to be adapted to newer variants as they come,” Goldman-Israelow says.