This year’s flu season is shaping up to be a nasty one—driven by a new variant of the influenza virus that may be able to slip past our vaccine defenses.
A mutated form of the influenza A strain H3N2 known as subclade K is causing a severe flu season in multiple countries across the world, including the U.K., Canada and Japan, and propelled a bad flu season in Australia. Now U.S. officials say it is driving up cases and hospitalizations here, too.
“Right now we’re seeing clade K everywhere we are seeing influenza” in the U.S., said Andrew Pekosz, a professor and vice chair of the department of molecular microbiology and immunology at the Johns Hopkins Bloomberg School of Public Health, in a press conference today.
On supporting science journalism
If you're enjoying this article, consider supporting our award-winning journalism by subscribing. By purchasing a subscription you are helping to ensure the future of impactful stories about the discoveries and ideas shaping our world today.
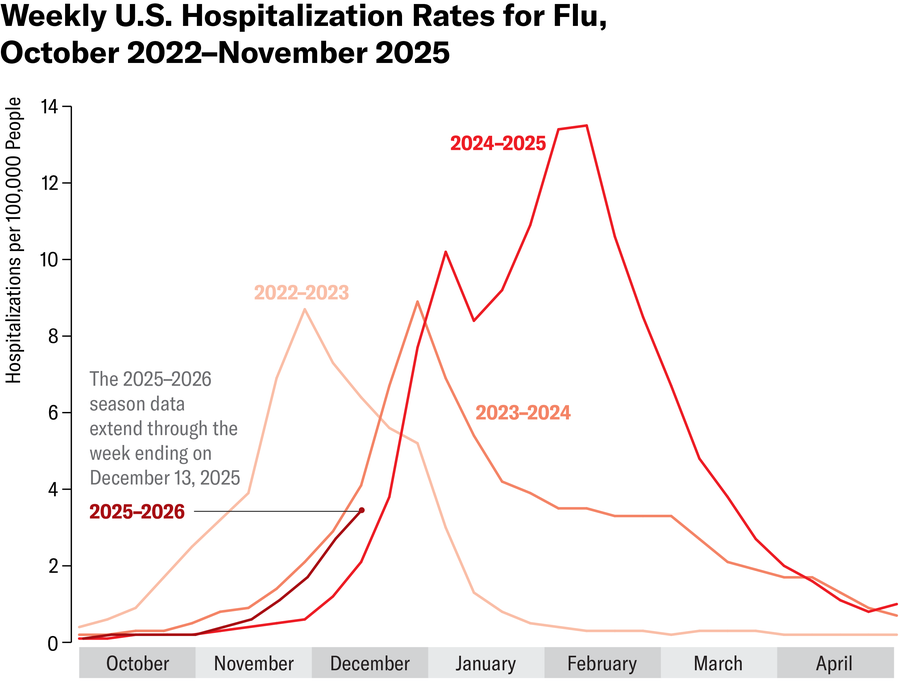
Amanda Montañez; Source: Centers for Disease Control and Prevention (data)
Worryingly, the mutations in the subclade K variant may make this year’s flu vaccine less effective. But experts say the shot, which was developed months before the new variant was identified, should still provide some protection against severe disease and death. The mutations “may allow it to evade some but not all of the influenza-vaccine-induced protection,” Pekosz explained.
“We’re still in the middle of trying to figure out whether it’s producing worse illness or whether what we’re seeing is a large number of cases that are increasing, and then there’s a correspondingly similar increase in terms of the severe illness,” he said.
Flu viruses are constantly evolving, but often these changes are relatively minor—a process known as antigenic drift. But sometimes a virus undergoes an evolutionary leap, or antigenic shift—and that can trigger a pandemic. Subclade K, while a significant change, is still considered to have undergone antigenic drift.
“The emergence of the new H3N2 influenza [subclade K] is concerning, as this variant emerged following development of the current-year influenza vaccine,” says physician Robert Hopkins, medical director of the National Foundation for Infectious Diseases. “But influenza is difficult to predict.”
The most recent update from the U.S. Centers for Disease Control and Prevention for the week ending on December 13 noted that flu infections are picking up across the country. Right now 17 jurisdictions are seeing high or very high influenzalike illness activity, and there have been two confirmed flu-related child deaths. But it’s still early in the flu season, which, in the U.S., typically starts in October and may not peak until February. Recent data indicates that nearly 90 percent of flu viruses sampled since September 28 belonged to subclade K.
Cumulative hospitalization rates, at 11 cases per 100,000, are already higher than this time last year. Texas is among the places that has seen an uptick in hospitalizations—potentially driven by the new variant—especially in those aged 65 and older.
The 2024–2025 flu season was one of the most severe in recent decades. While it’s rare to have back-to-back bad flu seasons, it’s not unheard of. And while this year’s flu shot may not be a perfect match for subclade K, the vaccine should still provide protection—even in those who are infected with the new variant, Hopkins says.
“It is not too late to get a flu shot,” Pekosz said at the press conference.
Additional reporting by Lauren J. Young.
Editor’s Note (12/16/25): This article was edited after posting to correct the number of states that are seeing high or very high influenzalike illness activity and to better clarify the descriptions of the subclass K variant and the U.S.’s cumulative influenza hospitalization rates for the week ending on December 6.
Editor’s Note (12/22/25): This article was update to include context about why the planned HHS announcement was delayed.

