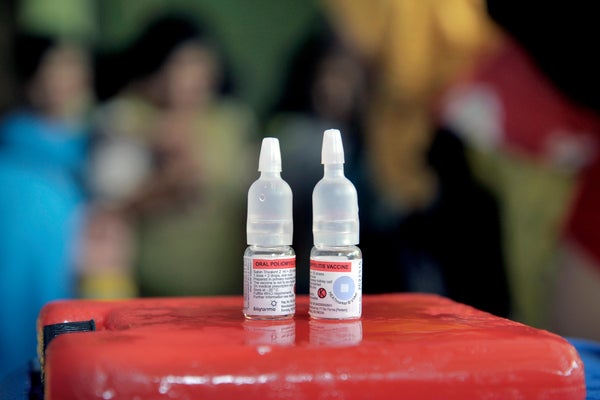
The discovery of poliovirus in New York state, London and Jerusalem this year has taken many by surprise — but public-health researchers fighting to eradicate the disease say it was only a matter of time.
“No country in the world is immune to the effects of polio,” says Zulfiqar Bhutta, a global-health researcher at the Aga Khan University in Karachi, Pakistan. “It’s all interconnected.”
The virus found in these regions is derived from an oral polio vaccine used in some countries. So far, only two cases of polio-related paralysis have been reported, in Jerusalem in February and New York in June; the New York infection was the first such US case in nearly a decade. But wastewater samples in all three areas suggest that the virus is circulating more widely.
On supporting science journalism
If you're enjoying this article, consider supporting our award-winning journalism by subscribing. By purchasing a subscription you are helping to ensure the future of impactful stories about the discoveries and ideas shaping our world today.
Polio causes irreversible paralysis in less than one in 200 of the susceptible people it infects, so the cases of paralysis suggest that many other people there have been infected, says Walter Orenstein, who studies infectious diseases at Emory University in Atlanta, Georgia. “Cases like that are just the tip of the iceberg,” he says. “It’s very concerning.”
Nature talked to researchers about the scale of the outbreak, and what can be done to stop it.
Why are these outbreaks happening?
Wild poliovirus circulates in only two countries — Afghanistan and Pakistan — where this year nine cases had been reported by June.
But vaccine-derived poliovirus appears periodically elsewhere, particularly in Africa and Asia. These cases come from a widely used oral vaccine that contains live, weakened virus that sometimes mutates to a dangerous form capable of infecting the nervous system.
Neither the United States nor the United Kingdom use that vaccine, opting instead for an injectable vaccine containing inactivated virus. This vaccine can keep the virus from infecting the nervous system, but it is not as effective as the oral virus at reducing viral shedding and halting transmission, says Raul Andino-Pavlovsky, a microbiologist at the University of California, San Francisco.
High polio vaccination rates in the United Kingdom, Israel and the United States mean that most children will be spared the virus’s worst effects (about 94% of US 5- and 6-year-olds are vaccinated). But unvaccinated people are vulnerable to the illness.
“This virus is very, very good at finding unvaccinated individuals,” says Orenstein. In the 1990s, a poliovirus outbreak in the Netherlands established a foothold in a community with a relatively low vaccination rate, despite the country’s overall vaccination coverage of more than 90%, says Oliver Rosenbauer, a spokesperson for the Global Polio Eradication Initiative of the World Health Organization (WHO) in Geneva, Switzerland. The outbreak resulted in 2 deaths and 59 cases of paralysis, and occurred 14 years after the country’s last endemic case of polio.
Has poliovirus spread beyond the regions where it was first identified?
Wastewater surveillance for polio is rare in rich countries; the United Kingdom routinely monitors sewage for the disease only in London and Glasgow. And New York began testing waste water in July, after officials learnt about the case of polio-related paralysis.
So it’s unclear how far the virus might have spread. But there is reason to hope that it hasn’t gone far: in London, which has been detecting poliovirus in sewage since February, the virus seems to have remained concentrated in the city’s north and east, and there have been no reports of polio-related paralysis. “It appears to be fairly localized, even within London,” says infectious-disease epidemiologist Nicholas Grassly at Imperial College London.
In New York, the virus has been detected in two counties as well as New York City, a geographical spread that is “very concerning”, says Orenstein. “It suggests we have had substantial transmission.”
The US Centers for Disease Control and Prevention (CDC) will prioritize wastewater surveillance for polio in under-vaccinated communities linked to the paralysis case. “Poliovirus testing from wastewater samples is very labour- and resource-intensive,” a CDC spokesperson told Nature. But surveillance systems set up to monitor the coronavirus SARS-CoV-2 are working to provide support, she added.
Can the outbreaks be contained?
The United States, Israel and the United Kingdom are all boosting vaccination efforts, which should fill gaps created during the COVID-19 pandemic. This includes an ambitious effort to vaccinate all one-to-nine-year-olds in London.
This strategy should nip the outbreaks in the bud, says Grassly. But the campaigns in London and New York will use injectable vaccine, so they will not stop virus transmission.
If, in six months or so, wastewater testing suggests that poliovirus has continued to spread, it might be necessary to look at other options, he says. For example, in 2020, the WHO listed a new oral polio vaccine for emergency use.
This vaccine contains weakened poliovirus. But researchers used knowledge of the virus’s genome — including how an error-prone enzyme involved in replicating the genome can generate genetic changes — to create a suite of mutations that keep the virus from regaining its ability to infect the nervous system. “It’s like putting the virus in an evolutionary cage,” says Andino-Pavlovsky, who helped to design the vaccine.
That vaccine has not yet undergone large-scale human testing, and has not been approved by UK or US regulators. But more than 100 million people have received it, says Andino-Pavlovsky, with no signs of vaccine-derived poliovirus emerging.
What is the status of polio outbreaks elsewhere?
Outbreaks in wealthy countries get lots of attention, says Rosenbauer. “But over the past 20 years, we’ve had many, many serious outbreaks around the world in developing countries.”
Rosenbauer says there are encouraging signs that the battle to eradicate polio is making progress, despite the disruption caused by COVID-19. Outbreaks in Yemen and a few countries in Africa are still active, he says, but their range is shrinking.
In places where there is armed conflict, such as areas of Afghanistan and Yemen, vaccination is difficult. “We need the political will to implement a plan to reach all the children in challenging areas,” he says. Otherwise, “the disease will come back globally”.
This article is reproduced with permission and was first published on August 22 2022.