For many people, a car is simply a way to get around. Drive it, fill the tank now and then, and when it breaks down, take it to the shop. When it wears out, trade it in for a new one.
This breezy attitude is fine for cars but a lousy way to run healthcare. Yet that is how medicine has worked in the U.S. for years. When we get sick, we go to the doctor for a fix. The problem is, when our bodies wear out, we can’t trade it in for a new one.
The reactive approach that has characterized U.S. healthcare for decades has worn thin. It is no longer economically sustainable. It has created a situation where more people spend a greater number of years suffering from chronic disease than ever before. As a result, there is a growing movement toward a proactive medicine that focuses on keeping body and mind healthy into old age—increasing healthspan, or years lived in good health, to something closer to lifespan. It’s a maintenance program of sorts for the one body you’ll ever have.
Healthspan medicine is a work in progress. There is no definitive how-to guide or protocol to follow. We need further discussion among clinicians, researchers and policymakers, as well as advances in the technologies at our disposal. However, many of the basic tenets are beginning to take shape. These include a focus on early detection through advanced screening and diagnostics, a recognition of the interconnectedness of human biology as a system of systems and understanding the critical role that aging biology plays as a root factor for most causes of disability and death.
At Optispan, the healthcare technology company I lead, we are developing a best-in-class healthspan medicine program called The Praxis (Latin for “practice”). Our goal is to enable access to rigorous, science-based health optimization for as many people as possible, ultimately scaling it to the point where it becomes a mainstream approach to healthcare. The upside is that millions of people will be able to preserve their vitality for many years, even decades, that might otherwise have been compromised by chronic disease. Many challenges remain, but our work is showing that it may be possible to create a future where a longer life is synonymous with a better one.
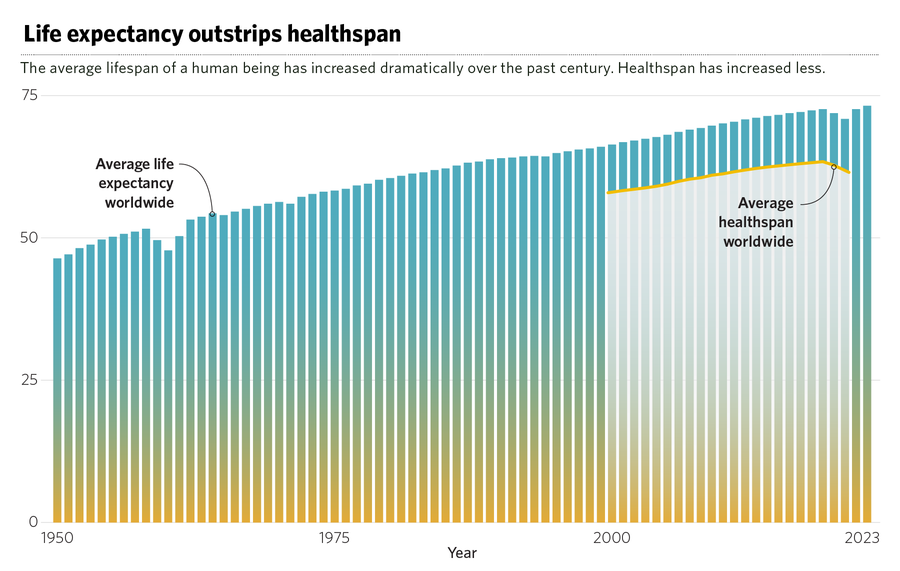
Katie Peek and Joelle Bolt; Sources: Life expectancy: UN World Population Prospects; healthspan: WHO; data for 2000-2021.
A gateway to prevention
Fundamentally, healthspan medicine is about determining where each person is on their health journey and helping them improve their trajectory. First, it is necessary to establish current health status as comprehensively as possible. We introduce the patient to the concepts of healthspan medicine through a “gateway experience,” which includes extensive evaluation.
Ideally, a single clinical site would have all necessary equipment and personnel to carry out the gateway experience in a single day, though this isn’t essential. This gateway day collects essential patient information and has a strong psychological and emotional impact—it marks the beginning of a lifelong journey. Afterwards, we follow up with regular coaching and biomarker updates. These provide ongoing support and metrics to evaluate progress and monitor for early signs that could lead to disease.
At the foundation of healthspan medicine are the pillars of health. These are easily understood through four simple verbs: eat, move, sleep and connect. These words encompass the ideas that nutrition and diet, which include eating healthy food in the right amounts; getting regular physical exercise and quality sleep; and maintaining balance through mindfulness and human relationships, are all necessary for optimal health. These fundamental lifestyle factors currently offer the greatest opportunities to expand healthy longevity and delay disease.
Many primary-care clinicians recognize how important these pillars are to their patients’ health and well-being. But doctors are often reluctant to advocate lifestyle changes because they’re considered too hard to act on. When doctors do address them, they generally give fragmented, outdated and one-size-fits all recommendations. In a rigorous healthspan medicine practice, doctors and coaches evaluate these pillars with a combination of patient-reported information, physiological biomarkers, functional assessments and wearable devices for continuous monitoring. They identify opportunities for improvement and develop a personalized health optimization program.
Effective healthspan medicine relies on regular feedback to the patient, which empowers and encourages self-determination. In our experience, this works best with a team that includes a medical professional, the patient and at least one coach or advocate—a new type of healthcare professional called the healthspan coach. At Optispan our healthspan coaches are trained in the principles and practices of health optimization. They have a working knowledge of systems medicine, geroscience principles and the pillars of health. They are informed about, and empowered by, the best technologies available to support behavior change, such as artificial intelligence tools. Coaches provide regular feedback, encouragement and strategies that support long-term health-promoting behaviors.
A systems medicine approach
Rather than focus on individual diseases in isolation, healthspan medicine relies on a systems biology framework to understand how the human body can function optimally. It considers health to be the balanced coordination of interconnected organs, tissues and cells. For simplicity, these are often categorized based on functions, such as cardiovascular, gut, hormonal, immune, skin, respiratory and musculoskeletal. Understanding how they interact with each other and using biomarkers—molecules that indicate how biological systems are functioning—allow us to detect early perturbations that might knock an individual’s health trajectory off course. These perturbations often suggest some corrective action we might take. In this way, we can identify each person’s highest risks and monitor the progress of mitigation strategies.
Geroscience, the scientific discipline linking biological aging with age-related functional declines, informs much of healthspan medicine. Major advances in geroscience over the past two decades have identified key mechanisms of aging, which have been formalized into twelve hallmarks, along with a growing understanding of the molecular networks that underlie, connect and regulate these hallmarks.
In recent years, new technologies have allowed for the development of high-dimensional molecular signatures of biological aging, or “clocks,” that appear to correlate with individual disease and mortality risk. While useful as research tools, clinical application of so-called biological aging clocks, particularly those marketed direct-to-consumer, should be approached with caution to avoid confusing patients and inducing unnecessary anxiety. In our experience, current biological age assessments may provide useful insights when used in combination with more established biomarkers, but they are not yet sufficiently validated for mainstream application.
The most effective approaches to slow biological aging are tightly coupled to the pillars of health (nutrition, exercise, sleep and connection). Estimates suggest that many people can gain more than a decade of healthspan simply by improving their pillars. There is also growing interest in drugs or supplements that can potentially mimic, or enhance, these lifestyle approaches. Preclinical studies have identified several “gerotherapeutics”—drugs that increase lifespan and healthspan in laboratory animals. Some of these studies provide indirect evidence for potentially similar benefits in humans. As a result, a small but growing number of practitioners are specializing in off-label prescriptions for putative “longevity” therapies such as rapamycin, metformin, SGLT2 inhibitors and other drugs.
Two additional classes of therapeutics worthy of mention here are hormone optimization strategies and GLP-1 anti-obesity drugs such as Ozempic, Wegovy and Mounjaro. These have seen a surge in popularity and a corresponding increase in the number of providers who are willing to prescribe them, including many who have co-opted the phrase “longevity medicine” without any real background knowledge or training in the field. While there is evidence that these therapies, when used properly, can enhance healthspan for many people (and perhaps even slow biological aging itself), there is also the potential for harm. For example, many patients lose significant muscle mass and bone density from GLP-1 agonists when prescribed in isolation, placing them at higher risk of frailty and potentially counteracting benefits attained in other domains. Such negative outcomes are largely preventable when use of these medications is approached through the framework of a holistic healthspan medicine program.
It is important to recognize that off-label use of pharmaceutical or natural products to slow biological aging is currently highly speculative. Their risk-versus-reward profiles are evolving with new data, and few definitive biomarkers are available to evaluate individual efficacy. Given the growing appetite for access to these therapies, there is an urgent need to develop validated biomarkers and expert guidelines to help responsible practitioners in best meeting the needs of their patients.
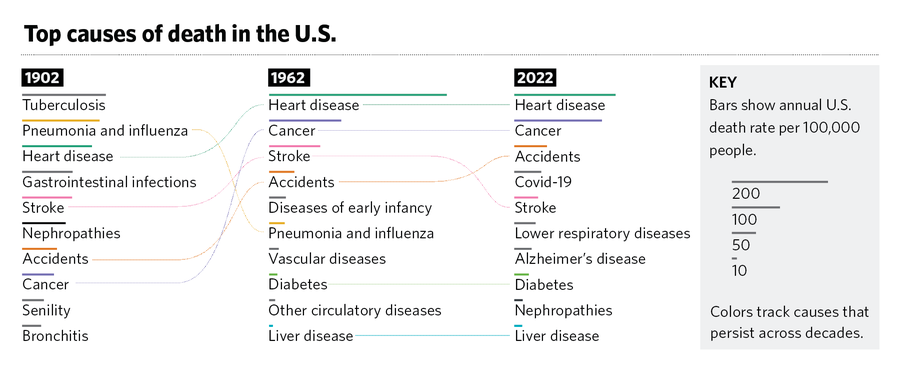
Katie Peek; Source: The National Center for Health Statistics
Opportunities and challenges
Widespread adoption of healthspan medicine has the potential to give most Americans 10 to 20 years of additional high-quality life. The social and economic dividends from recovering these lost decades are enormous. Indeed, a recent estimate from the McKinsey Health Institute calculated that for each year of increased healthy life, the U.S. would see $38 trillion in economic gain. While some will claim this kind of care is only for the rich, applying only a fraction of these gains would be sufficient to provide top-tier healthspan medicine to every man, woman and child in the U.S. For this to happen, however, at least two significant barriers must be overcome.
First, incentive structures will need to change to encourage aggressive preventative care. Such a change will require insurers, administrators and policymakers to recognize that keeping people healthy is ethically and economically superior to keeping people sick. In this regard, healthspan medicine is not a replacement for reactive disease care and need not threaten entrenched interests in the healthcare industry. Even with optimal prevention, people will still get sick. Yet, because healthspan medicine often detects problems early on, it provides opportunities for more effective treatments to halt or even reverse the trajectory of disease. This has the potential to alleviate stress on hospitals providing acute care and reduce the enormous burden of chronic disease.
Second, responsible stakeholders must align on a core set of values, standards and best practices. While a growing number of practitioners are embracing many of the concepts of healthspan medicine, the field remains fragmented and quality of care is uneven. Unfortunately, some self-identified longevity medicine providers prioritize cosmetic treatments, unproven experimental procedures or excessive reliance on supplements over evidence-based approaches grounded in rigorous science. Adding to the challenge, misinformation from online personalities and direct-to-consumer companies promoting questionable products has fueled skepticism and undermined trust in the field. To move forward, it is imperative that practitioners commit to ethical, transparent and science-driven practices. By fostering collaboration, self-regulation and accountability, the healthspan medicine community can elevate its credibility and unlock its potential.
We have an extraordinary opportunity to transform the quality and quantity of life for millions of people using the tools and knowledge available today. By reaching a consensus on protocols and approaches rooted in rigorous science and clinical best practices, the field of healthspan medicine can inspire confidence among patients and the broader medical community. As this vision takes shape, healthspan medicine has the potential to become a cornerstone of modern healthcare—ensuring that longer lives are not just possible, but also vibrant and fulfilling. With collaboration, innovation and a shared commitment to proactive care, we can create a future where everyone has the opportunity to thrive at every stage of life.
Learn how Optispan is using science-based preventive medicine to keep people healthy for as long as possible.
Explore the emerging science of healthspan in other stories in this special report.




