Around the fourth century BCE, the Greek physician Hippocrates postulated that good health is a balance between internal bodily fluids and external factors, such as the environment and lifestyle. His theory also holds true for the relationship between oral health, disease and bacteria.
Researchers have long assumed a connection between oral and general health, but they only began to explore it broadly in the 1990s. They found that periodontal disease results from a complex interplay between oral bacteria and the innate and adaptive immune responses. Moreover, they found the relationship can extend beyond the mouth, potentially contributing to or exacerbating certain systemic diseases.
In 2012, the American Academy of Periodontology (AAP) and the European Federation of Periodontology (EFP) brought together more than 70 leading researchers to make sense of the growing body of research. They focused primarily on the connection between periodontitis and cardiovascular disease (CVD), diabetes and adverse pregnancy outcomes, finding that associations indeed exist. Since then, evidence has only continued to mount, with more than 700 studies published that link periodontal diseases to systemic conditions.
Periodontist, Aaron Biesbrock, a Senior Director at Procter & Gamble’s Health Care Research Center, says that when he started out in dentistry, he was skeptical that associations existed. Now he is more convinced. He says that periodontitis is a condition that develops over the long term. “This is not an overnight tsunami,” he says. “It’s the cumulative effects of chronic infection in your mouth that may have systemic consequences.”
Researchers have made progress in revealing the precise cellular and molecular mechanisms beneath this infection, but to understand them one must first understand the ecosystem that is the mouth.
An ecosystem unlike any other
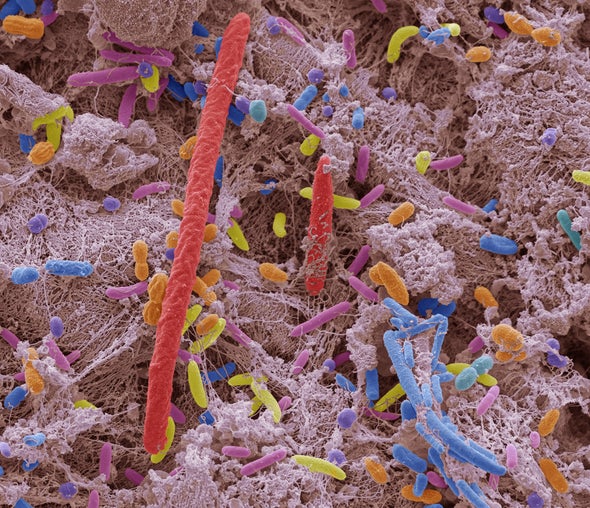
The bacterial colony, or oral microbiome, that populates the mouth is second only in size to the one in the gut. In a healthy mouth, bacterial species live in homeostasis, and they gather in dental biofilms, known as plaque, that accumulate throughout the mouth.
Trouble arises when homeostasis is lost. As plaque builds up, it can migrate below the gum line into an anaerobic environment, where certain pathogenic bacteria, notably Porphyromonas gingivalis, thrive. Those bacteria shed various cytotoxins, proteases and structural molecules. Along with chemical signals released by infected tissue, they spark an immune response. Neutrophils and macrophages are typically the first immune cells attracted to an infection. They attack bacteria by engulfing them while also secreting chemical signals that recruit other types of immune cells.

Immune responses typically resolve quickly if the plaque is removed. But in those susceptible to periodontitis—due to genetics, behaviours like smoking and poor nutrition or a systemic vulnerability—the inflammation becomes chronic.
When that occurs, tissues tend to break down, creating ulcerations under the gum line and pockets that allow anaerobic pathogens to flourish. The damage can spread to ligaments and bone supporting the teeth, causing deterioration and tooth loss.
Advanced periodontitis can also create conditions that drive systemic diseases. Ulcerations open a pathway for oral bacteria to enter the bloodstream, while chronic inflammation in the mouth can increase pro-inflammatory mediators in other parts of the body. Patients with periodontitis have demonstrated the presence of oral bacteria at sites throughout the body and elevated inflammation biomarkers, such as C-reactive protein.
Thomas Van Dyke, a professor of oral medicine at Harvard University and vice president of clinical and translational research at the Forsyth Institute, says inflammation evolved as a positive, protective response against infection. He believes periodontal disease is as much a failure of resolution as it is too much inflammation. If the inflammatory response goes unresolved, the cure, in essence, becomes the disease.
Links to systemic disease
Of the 57 possible systemic conditions currently being studied in connection with periodontal disease, diabetes has yielded the clearest evidence. Clinical studies show that among patients with poorly controlled diabetes, elevated levels of pro-inflammatory mediators and expression of Toll-like receptors within the gingival tissues contribute to increased periodontal destruction. Also, those with diabetes and periodontitis have significantly higher HbA1C levels, an indicator of blood glucose, than patients with diabetes alone.
According to Professor Iain Chapple, the head of research for the Institute of Clinical Sciences in Birmingham, England, the bidirectional relationship between periodontitis and diabetes is largely accepted. However, Chapple says, diabetes is far from the only disease that shows a connection to periodontal disease. “The oral-systemic interface is a big one for us,” he says. “All the studies that have been done on these different conditions show robust associations independent of the common risk factors.”
In one example, Chapple cites a recent a study of 770 patients with chronic renal disease which, as in studies of diabetic patients, demonstrates a bidirectional relationship. The results, recently published in the Journal of Clinical Periodontology, show periodontal inflammation and renal function are causally linked. The Birmingham team was able to show that a ten percent increase in periodontal inflammation resulted in a three percent decrease in renal function while a ten percent decrease in renal function resulted in a 25 percent increase in periodontal inflammation.
When it comes to an association between heart disease and periodontal disease, evidence exists, but it has not reached the level of a causal relationship. A consensus report from the European Federation of Periodontology and the World Heart Federation, published last year, confirms a positive association between periodontitis and CVD caused by bacteria moving into the circulatory system, promoting inflammation and hardening of the arteries.
But making the leap to true cause-and-effect could be difficult, Chapple says. “There is some evidence that if you provide periodontal therapy to patients with heart disease you can improve their outcomes, but I don’t think we will ever have gold-star evidence as the trials required to prove this would be unethical to run.”
The situation is similar with adverse pregnancy outcomes. Studies involving women with periodontal disease have found periodontal pathogens translocated to the placenta, but how this could drive an adverse outcome is still not clear. Maria Geisinger, the director of advanced education in periodontology at the University of Alabama at Birmingham School of Dentistry, points out that pregnant women tend to be younger and many will have pregnancy-related gingival inflammation.
In one recent study, however, Geisinger treated women for gum disease in conjunction with their regular maternity visit. She reported a 50% reduction in preterm births and low birth-weight when compared with historical clinical trials.
Treatments today and tomorrow
Treatments for prevention of periodontal diseases are well delineated. Home hygiene combined with regular appointments at the dental office are imperative, Biesbrock says. Beyond that, non-surgical periodontal therapy is recommended, says Dr. Salme Lavigne, retired professor and director of the School of Dental Hygiene, College of Dentistry at the University of Manitoba, Canada and currently the Scientific Editor of the Canadian Journal of Dental Hygiene. Non-surgical periodontal therapy includes debridement of the root surface to remove both hard and soft deposits that occur within periodontal pockets.
In the future, other more targeted therapies could exist. Van Dyke, along with his Harvard colleague and immunologist Professor Charles Serhan, have been investigating agents that actively promote resolution of inflammation, namely specialised pro-resolving lipid mediators (SPMs), including lipoxins, resolvins, protectins and maresins. Animal studies have shown that it is possible to chemically simulate the positive effects of SPMs.
Van Dyke explains: “You can take a chronic inflammatory disease like periodontitis, add back the resolution molecule and disrupt the cycle of destruction and drive a return to homeostasis.” Work is underway to develop a synthetic compound to mimic this effect.
Rich Lamont, a professor in the Department of Oral Immunology and Infectious Diseases at the University of Louisville, Kentucky, has been probing the bacterial community itself for clues to treatments. By learning how microorganisms communicate within the biofilm, Lamont says, “We are starting to understand the physical and chemical messages which can either attract or repel. We want to be in a situation where we can recruit the organisms we want and get rid of the pathogens we don’t want and prevent the transition from healthy plaque to a disease-provoking plaque.”
Indeed, most new therapies will have to take into account that the mouth is a dynamic system and that the science will continue to evolve. “When we look at our entire understanding of the microbiome and how that shapes overall wellness, it’s been such a paradigm shift in my practice lifetime,” Geisinger says. “Instead of looking at discrete bacteria we are looking at commensal or dysbiotic biofilm. We should see our oral microbiome as a partner in our immune system and in our well-being.”
To learn more about the connections between oral and general health, visit the dedicated page from Crest + Oral-B.