A new generation of cancer therapies has emerged over the past few decades, including checkpoint inhibitors and chimeric antigen receptor (CAR) T-cell therapies that modify or directly use T-cells to attack cancer.1
These approaches have benefited certain patients, but cancer is clever, and it can evade and suppress therapies like these that employ the adaptive immune system—one of the two interdependent arms of the immune system. This is particularly evident in “cold tumors,” which lack infiltration or activation of anti-cancer immunity and do not typically respond to existing immune therapies.
Novel therapies, however, could boost the ability of immune cells to infiltrate tumors and kill cancer cells. These therapies employ a different branch of the immune system called innate immunity that can help overcome cancer’s ability to evade immune recognition early in an immune response. By leveraging both arms of the immune system, researchers could give modern medicine powerful new tools to fight cancer.
The dawn of immunology
The power of the immune system to fight disease has intrigued scientists for centuries. The earliest known reference to immunity goes back more than two millennia to the plague of Athens in 430 B.C., when the Greeks realized that people who had survived smallpox were not infected with the disease a second time.2
Fast forward 2,300-plus years to the last quarter of the nineteenth century, when Elie Metchnikoff, a Russian zoologist, identified cells that could engulf and destroy foreign pathogens, known as phagocytic cells. This discovery became the basis for immunology.3
What the Greeks and Metchnikoff observed, and what scientists continue to uncover, is the complexity of the human immune system.3 The first of the immune system’s two interdependent arms, the innate immune system, consists of a variety of cell types, including natural killer (NK) cells, macrophages and dendritic cells, that serve as an initial line of defense against threats. Innate immune cells exhibit rapid cytotoxic activity against foreign pathogens and malignant cells, and they have the capacity to launch a counterpart arm, the adaptive immune system. The T-cells and B-cells in this system have receptors that recognize specific foreign antigens, and they develop long-lasting immune memory to protect against future infections or cancers.
Researchers have modulated the adaptive immune system to develop therapies for cancer, infectious diseases and autoimmune conditions. And beginning decades ago, scientists realized that they could potentially treat different illnesses by utilizing innate immunity.
The role of interferons in harnessing innate immunity
One of the earliest identified keys to unlocking the power of innate immunity was leveraging interferons, a family of inflammatory proteins that detect threats and signal the immune system, causing the awakening of innate immunity and downstream adaptive responses. After they were discovered in 1957, researchers showed that interferons had antitumor activity, and others explored using them to treat diseases.4 To date, interferons have been used to treat several chronic infectious diseases, as well as certain hematologic malignancies and solid cancers.5
Although interferons produce meaningful clinical benefit for some patients, they can result in serious side effects. This has limited their broad utility and driven researchers to explore a more nuanced approach to safely stimulate innate immunity to treat cancer.5
The cancer immunity cycle
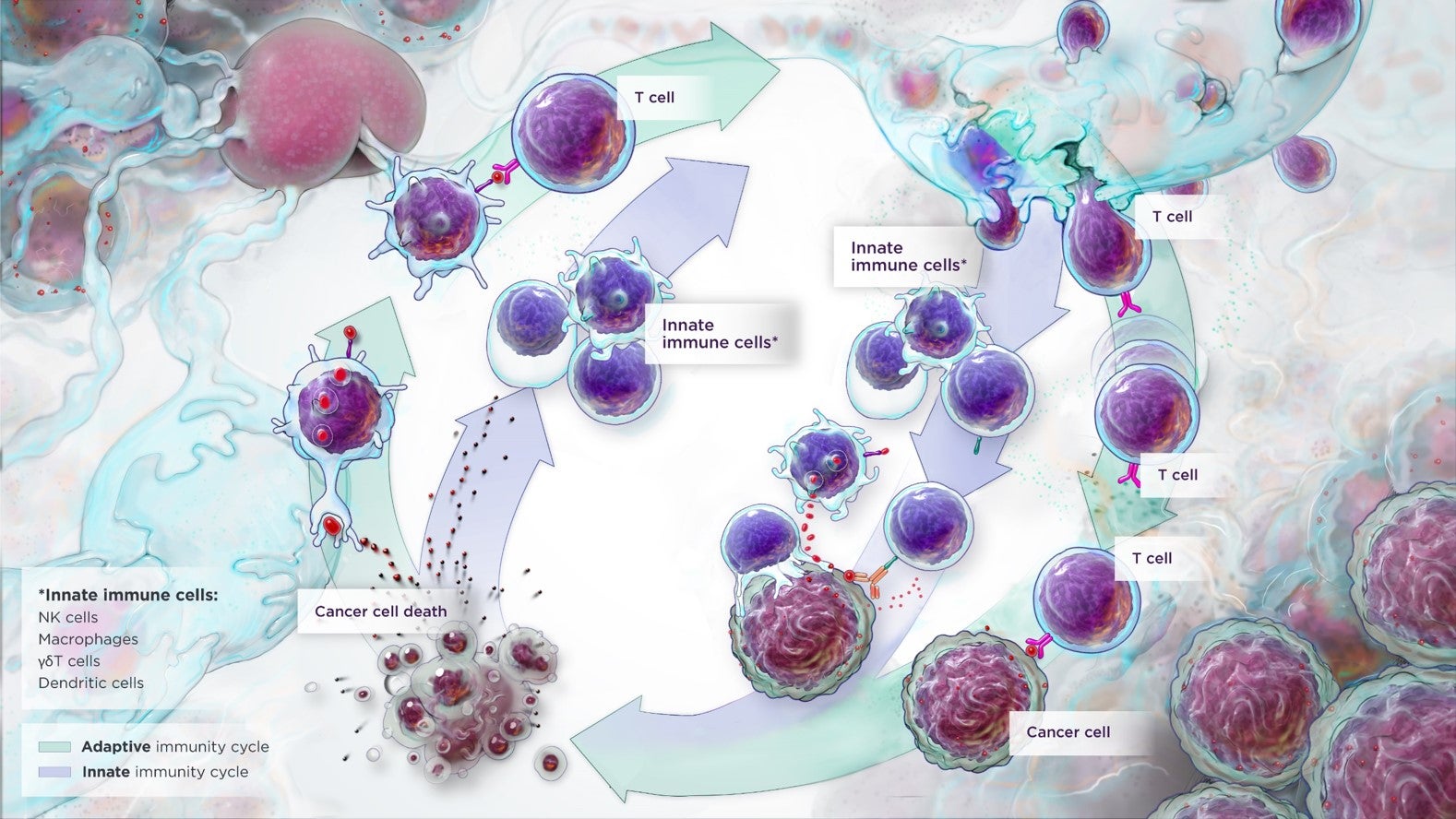
Our understanding of the immune system’s ability to recognize and attack cancer is best represented by what scientists refer to as “the cancer immunity cycle,” which maps the interplay between immune cells and tumors along key steps that, if productive, can lead to tumor eradication.6
The first steps in the cycle occur when specialized innate immune cells known as antigen-presenting cells are activated. This leads to triggering of the adaptive immune response through the presentation of cancer-derived signals (also known as antigens) to T-cells, typically in lymph nodes near tumor sites. These activated T-cells then migrate through blood vessels and infiltrate the tumor, subsequently killing the targeted cancer cells.7 Meanwhile, additional innate immune effector cells – including macrophages, NK cells and gamma delta (γδ) T-cells – are activated to directly attack and kill tumor cells upon contact, while critically shaping the overall tumor microenvironment to be more permissive to an effective immune response.
The future of cancer therapy
Today, researchers continue to explore how the innate immune system can outsmart cancer—work that has led to a steady increase of investigational therapies that harness innate immunity. For example, researchers at Takeda Oncology are exploring this emerging science through multiple programs that seek to address the needs of people living with cancer. These include therapeutics designed to tap into the power of interferons while avoiding the toxicities that have limited their use, cell therapies that leverage innate cell types such as NK cells and γδ T-cells, antibody-like molecules that engage immune cells to attack cancer cells, and other novel modalities.
By harnessing innate immunity, which helps to drive adaptive immunity, researchers aim to enhance a powerful immune defense mechanism that achieves a robust and durable attack on tumors at different tissue locations, thereby outsmarting cancer in ways never seen before.
To learn more about how innate immunity can be leveraged in cancer therapeutics, visit .https://www.takedaoncology.com/science-research/innate-immunity/.
References
- Grosser R, Cherkassky L, Chintala N, Adusumilli PS. Combination Immunotherapy with CAR T Cells and Checkpoint Blockade for the Treatment of Solid Tumors. Cancer Cell. 2019;36(5):471-482. doi:10.1016/j.ccell.2019.09.006
- Retief FP, Cilliers L. The epidemic of Athens, 430-426 BC. South Afr Med J Suid-Afr Tydskr Vir Geneeskd. 1998;88(1):50-53.
- Kaufmann SHE. Immunology’s Coming of Age. Front Immunol. 2019;10:684. doi:10.3389/fimmu.2019.00684
- Borden EC. Interferons α and β in cancer: therapeutic opportunities from new insights. Nat Rev Drug Discov. 2019;18(3):219-234. doi:10.1038/s41573-018-0011-2
- Friedman RM, Contente S. Interferons as Therapy for Viral and Neoplastic Diseases: From Panacea to Pariah to Paragon. Pharm Basel Switz. 2009;2(3):206-216. doi:10.3390/ph2030206
- Zhang X, Wang S, Zhu Y, et al. Double-edged effects of interferons on the regulation of cancer-immunity cycle. Oncoimmunology. 2021;10(1):1929005. doi:10.1080/2162402X.2021.1929005
- Chen DS, Mellman I. Oncology meets immunology: the cancer-immunity cycle. Immunity. 2013;39(1):1-10. doi:10.1016/j.immuni.2013.07.012