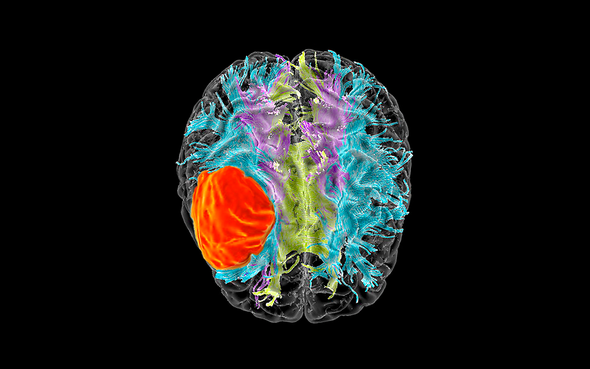
Of the more than 100 known cancers, glioblastoma, which occurs in the brain and spinal cord, is one of the most difficult to treat. Complete removal by surgery is impossible, while the most commonly used treatments for glioblastoma — radiation therapy and the chemotherapy drug temozolomide — are not very effective over the long term.

and the Director of the Brain Tumor Center at
Memorial Sloan Kettering Cancer Center.
Credit: Memorial Sloan Kettering Cancer Center
Researchers in the Brain Tumor Center at Memorial Sloan Kettering Cancer Center (MSK), led by developmental biologist Luis F. Parada, are focused on finding more effective ways to foil this deadly disease. In a recent study published in Nature, researchers from MSK and the University of Texas Southwestern Medical Center identified a compound that kills glioblastoma by targeting a cell type, cancer stem cells, often overlooked in traditional drug discovery. The compound disrupts cellular metabolism, effectively starving target cells of energy.
The findings are preliminary, and while the drug is not yet ready to be studied in clinical trials, it potentially points to a new method of treating glioblastoma and, perhaps, a number of other cancers.
A new view on glioblastoma leads to a killer compound
The insight behind the research is that tumors are composed of different kinds of cells while most drug discovery is based on homogenous cell lines.
“The pharmaceutical industry has traditionally used established cancer cell lines to screen for new drugs, but these cell lines don’t always reflect how cancer behaves in the body,” explains Dr. Parada, whose lab is in the Sloan Kettering Institute’s Cancer Biology and Genetics Program. As a result, certain cell types important for cancer growth—namely cancer stem cells—may not be included in the typical drug discovery process.
To get a clearer view of glioblastoma, investigators in Dr. Parada’s lab genetically engineered mice certain to develop the cancer, and then pooled cells from those tumors to create drug discovery panels. Their hope was this heterogeneous population of cells would be more accurate than traditional cell lines in reflecting the range of cell types making up a typical tumor.
Using high-throughput screening, a method in which hundreds of thousands of compounds can be rapidly evaluated, the researchers searched for candidates that could kill glioblastoma tumor cells, including cancer stem cells, without killing normally dividing cells. They started with a list of 200,000 compounds, which they then whittled to 5,000 then 2,000 then 60. More in-depth studies were conducted on the 60 most promising compounds.
One drug — which the team eventually dubbed Gboxin, short for “glioblastoma toxin” — rose to the top. It was effective at curbing the growth of glioblastoma tumors in mice and did not seem to make them sick.
“Once we identified this compound, the next step was to test it on glioblastoma cells derived from patients with glioblastoma,” Dr. Parada says. “We found that the human glioblastoma cells all succumbed to Gboxin.”
After the researchers showed that Gboxin was effective at treating glioblastoma in mice and killing human glioblastoma cells, they set out to determine how and why it worked.
An unexpected mechanism opens up new possibilities for treatment
Clues to Gboxin’s mechanism came from its unique ability to target cancer stem cells. Like normal stem cells, cancer stem cells can give rise to many other types of cells. This means they have the ability to rebuild a tumor, even after most of it has been removed, leading to cancer relapse and metastasis.
Because cancer stem cells don’t behave like typical tumor cells, they don’t share the same vulnerabilities. “The therapies that are currently in use were designed to target cells that are rapidly dividing,” Dr. Parada says. “But what we’ve concluded in our studies is that glioblastoma stem cells divide relatively slowly within tumors, leaving them unaffected by these treatments.”
The researchers found that Gboxin killed cancer stem cells by affecting a specific component of their metabolism and starving them of energy. Specifically, Gboxin appears to prevent cells from making ATP — the cell’s energy currency — by interfering with oxidative phosphorylation, a process that occurs in cellular structures called mitochondria, the cell’s energy factories.
“Stem cells are very specialized and need a lot of energy to do their thing,” Dr. Parada says. “When Gboxin accumulates within cancer cells, it essentially strangles the mitochondria and shuts energy production down.”
Other dividing cells in the body, including other cancer cells, rely less on oxidative phosphorylation than stem cells. They employ instead glycolysis, a metabolic process better suited to generating the building materials required for new cells. The difference makes them much less sensitive to Gboxin.
“Ideally, what we want in a glioblastoma drug is something that targets the cancer stem cells specifically, while sparing normal cells.” Dr. Parada says. “That’s what Gboxin seems to do.”
The next steps for Gboxin
There is still much work to do before Gboxin can be tested in clinical trials in humans. The investigators need to determine that Gboxin can cross the blood-brain barrier. If not, they’ll need to develop a similar compound that can. They will also need to test the compound for potential side effects.
Dr. Parada says that because many tumors develop from cancer stem cells, the findings about Gboxin and glioblastoma stem cells may be applicable to other types of cancer. “What we know about cancer stem cells in general suggests that they all use similar mechanisms for their growth and proliferation,” he concludes. “If this drug turns out to be effective against glioblastoma, we’ll be very happy. If it turns out to work against other types of cancer, that would be great, too.”
To learn more about the latest in cancer research and treatment visit Memorial Sloan Kettering Cancer Center.