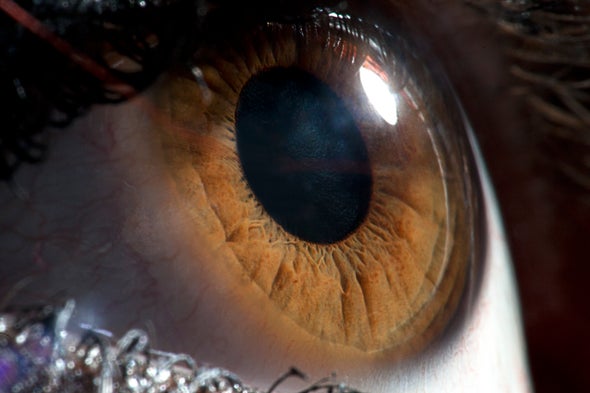
Battlefield and emergency room surgeons must combine skill and speed to treat eye injuries. This takes practice with realistic model eyes. Thanks to advances in 3-D medical printing at the Uniformed Services University of the Health Sciences (USUHS), and Walter Reed National Military Medical Center, those models have graduated from plastic to biological materials.
“We’ve seen significant improvements with our 3-D printing that haven’t been equaled outside the military,” says Vincent Ho, who heads USUHS’s Center for Biotechnology (4D Bio3) and is a leader in deploying 3-D printing for clinical use and training. Ho is also chief of radiology at Walter Reed, where he completed his medical training and U.S. Army service.
Realistic practice runs
Ho’s and collaborators from Walter Reed and other institutions began by printing low-cost polyolefin plastic replicas to train military physicians to remove shrapnel and debris with minimal damage to the organ itself. The model itself featured a face with removable 3-D printed eyeballs, each fitted with a silicone lens.
Ho’s models were more realistic and affordable than their commercial counterparts, but they were still plastic. Building on that, 4D Bio3 became one of the first labs to introduce tissue engineering into surgical simulation. It pioneered electrospinning nanofibers of collagen, the most common mammalian protein, over an extruded supporting gel to mirror the microstructure and tensile strength of a real human cornea. The team also incorporated reflective microbeads in the tissue, then recorded videos to provide ophthalmologists with precise feedback on how well they sutured the cornea during simulations.
“It was important to be able to modify bioprinted tissue to make it representative of the actual experience of surgery,” Ho says. “With this model, surgeons [in USUHS’s Tri-Service Ocular Trauma Course] get sensory feedback when they cut, with a feeling of depth or pressure on their scalpel.”
Printing human tissue
Ho and his colleagues are also pursuing other projects, including attempts to 3-D print tissue to replace missing or damaged body parts. The team also hopes to develop engineered human blood products that could be created during military operations instead of relying on blood from distant donors.
The technology has already been used to successfully 3-D print human meniscus tissue, the cartilage between the surfaces of the knee. The study was conducted in an African desert setting and reflects what military physicians would face in the field. Similar experiments are being planned to conduct medical 3-D printing in jungle, aquatic, arctic and high-altitude settings.
The work satisfies Ho’s long-term goal of pushing scientific boundaries while helping service members and veterans. “They risk their lives for us and deserve the best care we can give them,” he says. “Medical 3-D printing has a large role to play in that.”
To explore careers in the U.S. Army Medical Department (AMEDD), click here.