In 1900, a U.S. Army medical team led by Major Walter Reed proved that mosquito bites infected people with yellow fever. More than a century later, scientists at the Walter Reed Army Institute of Research are working on a single treatment for two dangerous mosquito-borne viruses, dengue and Zika.
The work grows out of a program at Walter Reed’s Emerging Infectious Diseases Branch, which aims to speed the development of treatments and vaccines. The COVID-19 pandemic has underscored the program’s importance.
“If there’s a new outbreak, we just don’t have the kind of time that it takes to create vaccines and treatments in traditional ways,” says Shelly Krebs, who joined the U.S. Military HIV Research Program to work on HIV vaccine development in 2012. Her work there helped her better understand how the immune system produces antibody-making B cells. Her goal is to use this knowledge to translate bench research on viral vaccines into successful treatments.
Zeroing in on Zika
Zika was first identified in monkeys in 1947, but it did not impact humans until an outbreak that began on Yap Island in the western Pacific in 2007, and reached Brazil in 2015. By 2016, the World Health Organization had categorized Zika, which causes neurological problems and birth defects, as a public health emergency of international concern.
Dengue is a widespread mosquito-borne tropical disease caused by the dengue virus. In most cases dengue is characterized by mild flu-like symptoms, but in rare instances can cause life-threatening complications such as rapid breathing and persistent vomiting.
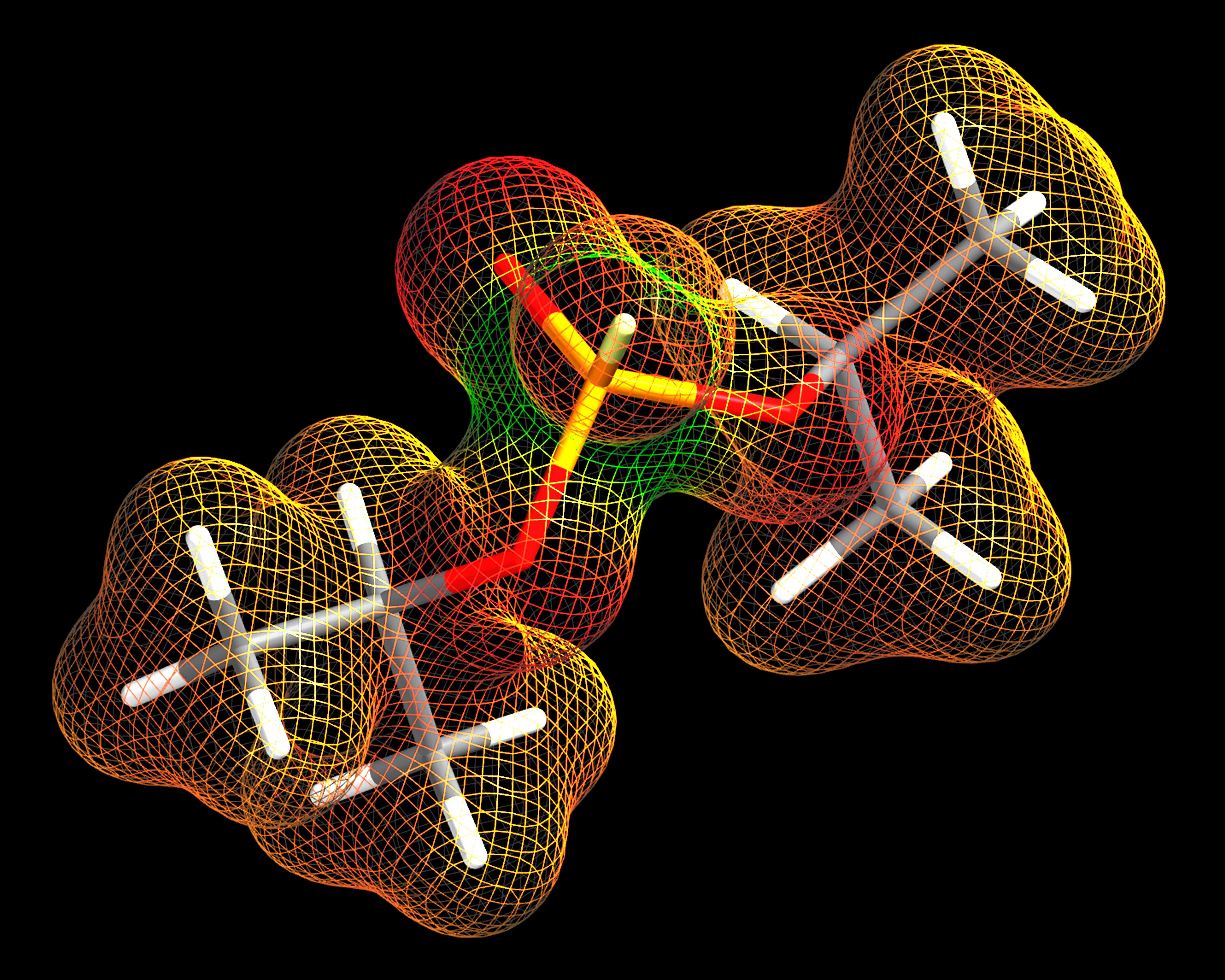
Zika and dengue belong to the same family of viruses—flaviviruses—and are chemically and structurally similar. This prompted Krebs and her colleagues to ask whether infection with one virus would affect how someone reacts to the other.
The majority of people in tropical regions have been exposed to dengue at some point in their lives, and Krebs vaccinated some of those individuals with a vaccine composed of inactivated Zika virus. It was not entirely a surprise when the subjects responded by producing antibodies that target both viruses, she and her colleagues reported last year in Nature Medicine.
These antibodies, called cross-neutralizing antibodies, recognize similar structures, or epitopes, that are shared among different viruses. “Cross-neutralizing antibodies are really important to identify,” Krebs says, because they can prevent and even treat infections by either virus.
Krebs’s team then produced cross-neutralizing monoclonal antibodies that could serve as a treatment for either disease. One of those monoclonal antibodies was able to neutralize both Zika and dengue at very low concentrations—just 10–20 nanograms per milliliter of blood. An antibody like that could be used as a treatment for someone who was infected but not previously vaccinated.
Advancing immunity in soldiers
“One of the main messages from this work is that the outcome really depends on the person’s background exposure,” Krebs says. Soldiers who have not been exposed to dengue or Zika would need to be vaccinated against both. But soldiers previously exposed to dengue could be protected against both after one vaccination. “This kind of information helps us make decisions going forward for our service members,” Krebs says.
This work goes beyond the medical needs of the U.S. Army. “Our work turns soldier health into world health,” Krebs says. “Everything we do for the soldier can translate into helping others around the world.”
To explore careers in the U.S. Army Medical Department (AMEDD), click here.